Your gut holds trillions of microscopic organisms that control far more than digestion. These bacteria influence your immune system, mental clarity, energy levels, and even your mood throughout the day. The gut microbiome serves as a command center for overall health.
This Website contains affiliate links. That means I may earn a small commission if you purchase through my links, at no extra cost to you.
Recent research shows that what you eat directly shapes which bacteria thrive in your digestive tract. A gut health diet provides the specific nutrients these beneficial microorganisms need to flourish. When your microbiome falls out of balance, inflammation rises and diseases take hold.
This comprehensive guide reveals exactly how food choices reshape your gut bacteria. You will discover which specific foods heal inflammation and which ones damage your intestinal lining. The science-backed strategies here offer practical steps anyone can implement today.
Understanding the connection between diet and gut health empowers you to take control of your wellbeing. Small dietary changes create massive shifts in how your body functions. Your journey to a healthier gut starts with the next meal you choose.
Understanding Your Gut Microbiome and Its Impact on Health
The gut microbiome consists of trillions of bacteria, viruses, fungi, and other microorganisms living primarily in your large intestine. These organisms outnumber your human cells by roughly three to one. Scientists now recognize this ecosystem as a vital organ that affects nearly every aspect of health.
Your microbiome weighs approximately two to five pounds and contains more genetic material than your entire body. Each person develops a unique microbial fingerprint based on birth method, early diet, antibiotic exposure, and ongoing food choices. This diversity determines how well your body processes nutrients and fights disease.
The Microbiome’s Role in Digestion and Nutrient Absorption
Beneficial bacteria in your gut break down complex carbohydrates that human enzymes cannot digest. They produce short-chain fatty acids during this process. These compounds provide energy to the cells lining your colon and reduce inflammation throughout your body.
The microbiome also manufactures essential vitamins including vitamin K and several B vitamins. Without adequate bacterial diversity, your body struggles to absorb minerals like calcium, magnesium, and iron. This explains why two people eating identical diets may experience vastly different nutritional outcomes.
Gut bacteria help regulate the immune system by training it to distinguish between helpful and harmful substances. Approximately seventy percent of your immune cells reside in the gut. A balanced microbiome prevents the immune system from overreacting to harmless food proteins or attacking your own tissues.
How Gut Health Influences Overall Wellness
The gut produces neurotransmitters including serotonin, dopamine, and GABA that regulate mood and cognition. About ninety percent of the body’s serotonin originates in the digestive tract. An imbalanced microbiome can contribute to anxiety, depression, and cognitive fog.
Research demonstrates clear connections between gut health and conditions like obesity, diabetes, heart disease, and autoimmune disorders. Chronic inflammation often begins in the gut when harmful bacteria outnumber beneficial species. This systemic inflammation contributes to the development of numerous chronic diseases.
Immune System Support
Beneficial bacteria train immune cells to respond appropriately to threats while maintaining tolerance to harmless substances in your environment and food.
- Produces antimicrobial compounds that fight pathogens
- Strengthens the intestinal barrier against toxins
- Regulates inflammatory responses throughout the body
- Helps prevent autoimmune reactions and allergies
Metabolic Regulation
The microbiome influences how your body stores fat, regulates blood sugar levels, and responds to hormones that control hunger and satiety signals.
- Affects insulin sensitivity and glucose metabolism
- Produces hormones that regulate appetite and fullness
- Influences cholesterol levels and fat storage
- Determines calorie extraction from food
Mental Health Connection
The gut-brain axis represents bidirectional communication between your digestive system and central nervous system through neural, hormonal, and immunological pathways.
- Manufactures neurotransmitters affecting mood
- Influences stress response and anxiety levels
- Impacts cognitive function and memory
- Affects sleep quality and circadian rhythms
Disease Prevention
A diverse, balanced microbiome protects against various diseases by maintaining intestinal integrity and regulating immune function across all body systems.
- Reduces risk of inflammatory bowel diseases
- Lowers likelihood of obesity and metabolic syndrome
- Decreases colon cancer risk through beneficial compounds
- Protects against cardiovascular disease and diabetes
Signs of an Unhealthy Gut Microbiome
Digestive symptoms like bloating, gas, diarrhea, or constipation often signal microbial imbalance. However, gut problems manifest in ways that seem unrelated to digestion. Skin conditions, frequent infections, fatigue, and mood changes can all stem from poor gut health.
Food intolerances that develop suddenly may indicate a damaged intestinal lining or bacterial imbalance. When harmful bacteria dominate, they can increase intestinal permeability. This condition allows partially digested food particles and toxins to enter the bloodstream, triggering immune reactions.
Unexplained weight changes despite consistent eating habits can point to microbiome dysfunction. Some bacterial species extract more calories from food than others. An overabundance of certain microbes may contribute to weight gain even when calorie intake remains stable.
How Diet Shapes Your Gut Microbiome
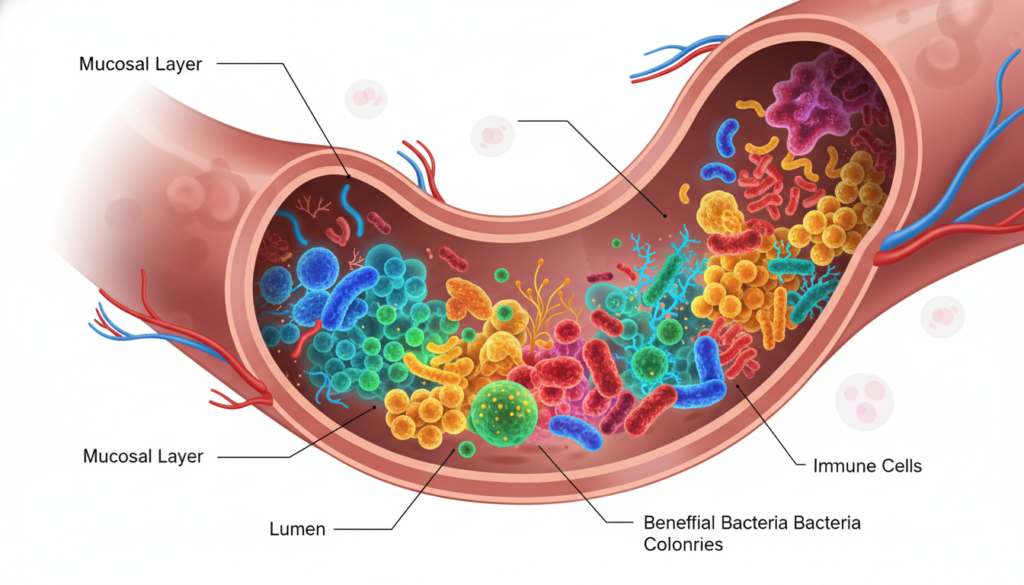
Every meal you consume feeds either beneficial or harmful bacteria in your gut. Different bacterial species thrive on specific nutrients. Your dietary choices over time determine which microorganisms multiply and which ones die off.
This process happens remarkably fast. Studies show that significant changes in gut bacteria composition can occur within just three to four days of dietary modification. A single week of eating more fiber dramatically increases populations of fiber-fermenting bacteria.
The Fiber Connection to Bacterial Diversity
Dietary fiber serves as the primary food source for beneficial gut bacteria. When these microorganisms break down fiber, they produce short-chain fatty acids like butyrate, propionate, and acetate. These compounds reduce inflammation, strengthen the intestinal barrier, and provide energy to colon cells.
Most Americans consume only fifteen grams of fiber daily, far below the recommended twenty-five to thirty-eight grams. This chronic fiber deficiency starves beneficial bacteria and allows harmful species to flourish. The diversity of fiber types matters as much as total quantity.
Different fibers feed different bacterial species. Resistant starch found in cooked and cooled potatoes or rice nourishes specific bacteria that produce high amounts of butyrate. Inulin from chicory root, garlic, and onions feeds Bifidobacteria species that support immune function.
Fermented Foods and Probiotic Bacteria
Fermented foods contain live beneficial bacteria that can colonize your gut. Regular consumption of yogurt, kefir, sauerkraut, kimchi, and other fermented products introduces diverse bacterial strains. These foods also provide the nutrients these bacteria need to survive the journey through your stomach acid.
Research indicates that people who eat fermented foods daily show greater microbiome diversity than those who avoid them. The beneficial bacteria in these foods produce compounds that inhibit pathogenic organisms. They also enhance the production of vitamins and improve mineral absorption.
Not all fermented foods offer equal benefits. Pasteurized versions contain no live bacteria. Check labels for terms like “live and active cultures” or “unpasteurized” to ensure you get viable microorganisms. Starting with small portions helps your system adjust to increased bacterial intake.
How Processed Foods Damage Gut Health
Ultra-processed foods contain emulsifiers, artificial sweeteners, and preservatives that harm beneficial bacteria. Emulsifiers like carboxymethylcellulose and polysorbate-80 erode the protective mucus layer in your intestine. This allows bacteria to reach the intestinal wall and trigger inflammation.
Artificial sweeteners including aspartame, sucralose, and saccharin alter gut bacteria composition in ways that promote glucose intolerance. These compounds selectively kill beneficial species while allowing harmful bacteria to multiply. Even small amounts consumed regularly can disrupt metabolic health.
High-sugar and high-fat processed foods feed bacteria that produce inflammatory compounds. These organisms thrive on simple sugars and create byproducts that damage the intestinal lining. Over time, this dietary pattern reduces bacterial diversity and increases disease risk.
The Diversity Principle
Bacterial diversity acts as a key marker of gut health. A diverse microbiome contains numerous species that perform different functions. This redundancy provides resilience against disturbances from antibiotics, illness, or dietary changes. Eating thirty different plant foods per week significantly increases microbiome diversity compared to eating fewer than ten plant varieties.
Protein Sources and Gut Bacteria
The type and amount of protein you consume influences which bacteria dominate your gut. Animal protein increases bacteria that produce trimethylamine N-oxide, a compound linked to cardiovascular disease when present in high levels. However, moderate amounts of lean animal protein provide essential amino acids without overwhelming these bacteria.
Plant proteins from legumes, nuts, and seeds come packaged with fiber and polyphenols that feed beneficial bacteria. These protein sources support the growth of bacteria that produce anti-inflammatory compounds. A diet emphasizing plant proteins tends to correlate with greater bacterial diversity.
Variety matters more than any single protein source. Rotating between different protein foods prevents overgrowth of bacteria adapted to specific proteins. This rotation strategy maintains balance and prevents any single bacterial group from dominating your microbiome.
Discover a Comprehensive Approach to Gut Health
While dietary changes form the foundation of gut health, understanding how to implement them effectively makes all the difference. Watch this free presentation from gut health experts who reveal how specific nutritional strategies, targeted supplementation, and lifestyle modifications work together to restore your microbiome. Learn the science-backed system that thousands have used to overcome digestive issues and reclaim their health.
Essential Foods That Heal and Nourish Your Gut
Specific foods provide exactly what beneficial gut bacteria need to thrive. These nutritional powerhouses contain fiber, polyphenols, and other compounds that selectively feed helpful microorganisms. Building meals around these foods transforms your microbiome composition.
The most effective gut health diet includes diverse plant foods consumed consistently. No single superfood creates lasting change. Instead, variety and regularity allow different beneficial bacteria to establish stable populations.
Fiber-Rich Vegetables and Fruits
Leafy greens like spinach, kale, and collards contain a unique type of sugar that feeds specific protective bacteria in the gut lining. These bacteria create a barrier against pathogens. Cruciferous vegetables including broccoli, cauliflower, and Brussels sprouts provide sulfur compounds that support detoxification and reduce inflammation.
Artichokes and asparagus deliver high amounts of inulin, a prebiotic fiber that Bifidobacteria species prefer. These vegetables also contain polyphenols that have antimicrobial properties against harmful bacteria while promoting beneficial species. Cooking these vegetables lightly preserves most of their prebiotic content.
Berries provide polyphenols that beneficial bacteria convert into anti-inflammatory compounds. Blueberries, raspberries, and blackberries contain anthocyanins that increase populations of bacteria associated with improved metabolic health. Fresh or frozen berries offer similar benefits.

Fermented Foods and Probiotic Sources
Yogurt and kefir contain Lactobacillus and Bifidobacterium strains that improve digestion and enhance immune function. Choose unsweetened versions with multiple bacterial strains listed on the label. Kefir typically provides greater bacterial diversity than yogurt and includes beneficial yeasts.
Sauerkraut and kimchi deliver Lactobacillus species along with fiber from the cabbage. These fermented vegetables survive stomach acid better than many probiotic supplements. Eating just two tablespoons daily provides billions of beneficial bacteria.
Miso, tempeh, and natto offer probiotics along with complete protein. These fermented soy products contain bacteria that produce vitamin K2, important for bone and cardiovascular health. Traditional fermentation methods preserve the most beneficial organisms.
Kombucha provides probiotics and organic acids that support gut health. Choose varieties with minimal added sugar, as excess sugar can feed harmful bacteria. The fermentation process should reduce sugar content significantly from the initial brewing stage.
Whole Grains and Resistant Starch
Oats contain beta-glucan, a soluble fiber that feeds bacteria producing anti-inflammatory compounds. Steel-cut or rolled oats preserve more of this beneficial fiber than instant varieties. Overnight oats create additional resistant starch as they soak.
Barley provides high amounts of beta-glucan and insoluble fiber. This grain supports bacteria that maintain healthy cholesterol levels. Pearl barley works well in soups and side dishes.
Cooked and cooled potatoes, rice, and pasta develop resistant starch that beneficial bacteria ferment into butyrate. This compound strengthens the intestinal barrier and reduces colon cancer risk. Reheating these foods maintains most of the resistant starch.
Quinoa and buckwheat offer complete protein along with diverse fibers. These pseudograins provide nutrients for a wide range of bacterial species. They work particularly well for people sensitive to wheat.
Legumes and Pulses for Gut Health
Lentils pack exceptional amounts of prebiotic fiber in a small serving. They contain resistant starch and oligosaccharides that feed beneficial bacteria. Red, green, and black lentils offer slightly different fiber profiles, so rotation increases bacterial diversity.
Chickpeas provide both soluble and insoluble fiber that support different bacterial populations. They contain galactooligosaccharides that specifically nourish Bifidobacteria. Cooking chickpeas thoroughly and eating them regularly helps reduce gas as your bacteria adapt.
Black beans, kidney beans, and navy beans deliver high fiber with polyphenols that have antioxidant properties. Soaking dried beans overnight and rinsing them reduces compounds that cause digestive discomfort. Adding seaweed like kombu during cooking further improves digestibility.
Daily Gut-Healing Food Targets
- Five to nine servings of vegetables, emphasizing variety
- Two to three servings of whole fruits, especially berries
- One to two servings of fermented foods
- Three servings of whole grains or resistant starch
- One serving of legumes or pulses
- Thirty different plant foods throughout the week
Starting Point for Beginners
If your current diet lacks fiber and fermented foods, increase intake gradually. Add one new gut-healthy food each week. Start fermented foods with one tablespoon daily, increasing slowly to avoid digestive upset. Your microbiome needs time to adapt to dietary changes. Sudden large increases in fiber can cause temporary bloating and gas as bacterial populations shift.
Nuts, Seeds, and Healthy Fats
Almonds contain prebiotic properties that increase beneficial Bifidobacteria and Lactobacillus populations. The polyphenols in almond skins provide additional food for these bacteria. Eating almonds with skins intact maximizes gut benefits.
Walnuts influence gut bacteria in ways that reduce inflammation and improve heart health markers. Studies show that regular walnut consumption increases bacteria that produce butyrate. Just one ounce daily provides meaningful benefits.
Flaxseeds and chia seeds deliver soluble fiber that becomes gel-like in your digestive tract. This gel feeds beneficial bacteria and helps maintain regular bowel movements. Grinding flaxseeds improves nutrient absorption.
Extra virgin olive oil contains polyphenols that increase beneficial bacteria while reducing harmful species. The oil also decreases intestinal inflammation. Choose high-quality, cold-pressed versions for maximum polyphenol content.
Herbs, Spices, and Polyphenol-Rich Foods
Turmeric and its active compound curcumin support beneficial bacteria growth while inhibiting pathogenic species. Curcumin also reduces intestinal inflammation directly. Combining turmeric with black pepper increases absorption significantly.
Ginger contains compounds that have antimicrobial properties against harmful bacteria while supporting beneficial populations. It also stimulates digestive enzyme production. Fresh ginger provides more active compounds than dried powder.
Garlic acts as a prebiotic feeding beneficial bacteria while fighting harmful organisms. Raw garlic contains allicin, a powerful antimicrobial compound. Crushing or chopping garlic and letting it sit for ten minutes before cooking preserves more allicin.
Green tea polyphenols selectively promote beneficial bacteria growth. Regular green tea consumption increases Bifidobacteria populations. The polyphenols also have direct anti-inflammatory effects on the intestinal lining.
Dark chocolate with at least seventy percent cacao contains polyphenols that beneficial bacteria convert into anti-inflammatory compounds. These bacteria break down cocoa flavonoids into smaller molecules that reduce inflammation throughout the body.
Foods That Damage Your Gut Microbiome

Certain foods actively harm beneficial bacteria while promoting the growth of problematic organisms. These dietary elements trigger inflammation, damage the intestinal lining, and reduce bacterial diversity. Eliminating or minimizing these foods allows your microbiome to recover and flourish.
The most damaging foods often appear innocuous or even healthy based on marketing claims. Understanding how specific ingredients affect gut bacteria helps you make informed choices. Even small amounts of certain additives can disrupt your microbiome.
Added Sugars and Artificial Sweeteners
Refined sugar feeds harmful bacteria and yeast species that produce inflammatory compounds. High sugar intake decreases beneficial Bifidobacteria while increasing bacteria associated with metabolic disease. Sugar also damages the intestinal barrier by promoting the growth of bacteria that break down the protective mucus layer.
Artificial sweeteners including aspartame, sucralose, and saccharin alter gut bacteria in ways that impair glucose metabolism. Studies demonstrate that these compounds reduce beneficial bacteria populations while increasing species associated with obesity and diabetes. Even occasional use can disrupt the microbiome balance.
High-fructose corn syrup damages gut bacteria differently than regular sugar. It promotes bacterial species that increase intestinal permeability. This allows toxins and partially digested food particles to enter the bloodstream, triggering systemic inflammation.
Emulsifiers and Food Additives
Carboxymethylcellulose and polysorbate-80, common emulsifiers in processed foods, erode the mucus barrier protecting your intestinal wall. These additives allow bacteria to reach and penetrate the intestinal lining. Animal studies show that regular emulsifier consumption promotes inflammatory bowel disease and metabolic syndrome.
Carrageenan, used to thicken many dairy alternatives and processed meats, causes intestinal inflammation and damages beneficial bacteria. This additive appears in many products marketed as healthy. Reading ingredient labels helps identify and avoid this problematic substance.
Maltodextrin, a common food additive and filler, suppresses beneficial bacteria growth while promoting harmful E. coli populations. It also impairs antimicrobial responses in the gut. This ingredient hides in protein powders, artificial sweeteners, and countless processed foods.
Excessive Alcohol Consumption
Regular alcohol intake reduces beneficial bacteria diversity and increases intestinal permeability. Even moderate drinking can allow bacterial toxins to enter the bloodstream. Alcohol also disrupts the balance between beneficial and harmful bacteria, favoring pro-inflammatory species.
Heavy drinking causes significant dysbiosis, characterized by overgrowth of potentially pathogenic bacteria. This imbalance contributes to liver disease progression. The damage extends beyond the gut, affecting the liver’s ability to filter toxins from the blood.
Occasional moderate consumption of red wine may provide some polyphenols that benefit gut bacteria. However, any potential benefits disappear with regular or heavy drinking. The negative effects on the microbiome outweigh any antioxidant advantages.
Red and Processed Meats
High consumption of red meat increases bacteria that convert carnitine and choline into trimethylamine. Your liver then transforms this into TMAO, a compound associated with increased cardiovascular disease risk. Plant-based eaters have very low TMAO levels even when they consume carnitine, suggesting their gut bacteria differ significantly.
Processed meats contain nitrates, nitrites, and other preservatives that harm beneficial bacteria. These additives also increase the production of harmful compounds during digestion. Regular consumption of processed meats correlates with reduced bacterial diversity and increased inflammation.
Charred or well-done meats create heterocyclic amines and polycyclic aromatic hydrocarbons. These compounds damage intestinal cells and alter gut bacteria composition. Cooking meat at lower temperatures and avoiding charring reduces these harmful substances.
The Antibiotic Problem in Meat
Conventionally raised livestock receive antibiotics that persist in meat products. These antibiotic residues can disrupt your gut bacteria even in small amounts. Choosing organic or antibiotic-free meat products reduces this exposure. The routine use of antibiotics in animal agriculture contributes to antibiotic-resistant bacteria that can colonize human guts.
Refined Grains and Low-Fiber Starches
White bread, white rice, and regular pasta lack the fiber that beneficial bacteria require. These refined grains cause rapid blood sugar spikes that feed harmful bacteria and yeast. The refining process removes the bran and germ where most fiber and nutrients reside.
Products made with enriched flour contain synthetic vitamins but remain devoid of the fiber, polyphenols, and minerals found in whole grains. Your gut bacteria cannot ferment these refined starches into beneficial short-chain fatty acids. Regular consumption starves beneficial bacteria.
Many gluten-free products rely heavily on refined rice flour and starches that offer no fiber. These alternatives often contain more sugar and additives than traditional wheat products. Choosing whole-grain gluten-free options like quinoa, buckwheat, and brown rice provides better gut health support.
Industrial Seed Oils and Trans Fats
Highly processed vegetable oils including soybean, corn, and cottonseed oil contain high levels of omega-6 fatty acids that promote inflammation when consumed in excess. These oils undergo chemical extraction and high-heat processing that creates harmful compounds. The imbalanced ratio of omega-6 to omega-3 fats in modern diets disrupts gut bacteria composition.
Trans fats found in partially hydrogenated oils damage gut bacteria and increase intestinal inflammation. Although banned in many countries, trans fats still appear in some processed foods. Check labels for “partially hydrogenated” oils and avoid these products completely.
Repeatedly heated oils, common in restaurant deep fryers, generate toxic compounds that harm gut bacteria. These oxidized fats damage the intestinal lining and promote growth of harmful bacterial species. Home cooking with fresh oils at appropriate temperatures minimizes this damage.
- Artificial sweeteners in diet products
- Emulsifiers in ice cream and processed foods
- High-fructose corn syrup in sodas and sweets
- Carrageenan in dairy alternatives
- Maltodextrin in protein powders and snacks
- Processed meats with preservatives
- Trans fats in baked goods
High-Risk Gut Disruptors
- Conventional dairy products with antibiotics
- Refined grains without fiber
- Regular alcohol consumption
- High-sugar fruits in excess
- Excessive red meat portions
- Industrial seed oils in cooking
- Fried foods from restaurants
Moderate-Risk Foods
Lifestyle Factors That Influence Gut Health
Diet forms the foundation of gut health, but other lifestyle factors significantly impact your microbiome. Sleep quality, stress levels, exercise habits, and medication use all shape which bacteria thrive in your digestive tract. These elements work synergistically with nutrition to determine overall gut health.
Addressing lifestyle factors creates an environment where beneficial bacteria can flourish even when dietary choices are not perfect. Conversely, poor lifestyle habits can undermine even the healthiest gut health diet. A holistic approach produces the most dramatic improvements.
Sleep Quality and Circadian Rhythms
Your gut bacteria follow circadian rhythms that influence metabolism and immune function. Irregular sleep schedules disrupt these bacterial cycles. Studies show that shift workers have reduced bacterial diversity and higher rates of metabolic disorders compared to people with regular sleep patterns.
Sleep deprivation alters gut bacteria composition in ways that increase inflammation and impair glucose metabolism. Just two nights of poor sleep can change your microbiome. Chronic sleep restriction promotes bacteria associated with obesity and insulin resistance.
The relationship works both ways as gut bacteria produce neurotransmitters and compounds that influence sleep quality. An unhealthy microbiome can contribute to insomnia and poor sleep. Improving gut health through diet often leads to better sleep, which further enhances the microbiome.
Aim for seven to nine hours of consistent sleep per night. Going to bed and waking at similar times daily helps synchronize your gut bacterial rhythms. Creating a dark, cool sleep environment and avoiding screens before bed supports both sleep quality and microbiome health.
Stress Management and the Gut-Brain Connection
Chronic stress dramatically alters gut bacteria composition through stress hormones and nervous system activation. Stress increases intestinal permeability, allowing bacterial toxins to enter the bloodstream. This triggers inflammation and further disrupts the microbiome.
The gut-brain axis allows bacteria to influence stress response and mental health. Some bacteria produce GABA, a calming neurotransmitter. Others manufacture compounds that increase anxiety. Stress reduction practices like meditation, deep breathing, and yoga improve gut bacteria diversity.
Social connection and positive relationships support healthy gut bacteria. Isolation and loneliness correlate with reduced bacterial diversity and increased inflammation. Regular social interaction appears to benefit the microbiome through multiple pathways including stress reduction.

Physical Activity and Exercise
Regular exercise increases beneficial bacteria diversity independent of diet. Physical activity promotes bacteria that produce short-chain fatty acids and reduce inflammation. Athletes show distinct microbiome patterns compared to sedentary individuals, even when controlling for dietary differences.
Moderate exercise stimulates beneficial changes in gut bacteria within weeks. Studies demonstrate that thirty to sixty minutes of aerobic activity most days increases Bifidobacteria and other beneficial species. The improvements reverse when exercise stops, indicating the need for ongoing activity.
High-intensity exercise can temporarily increase intestinal permeability during workouts. However, regular training strengthens the gut barrier over time. Proper nutrition around exercise and adequate recovery prevent negative effects.
Both aerobic exercise and strength training benefit gut bacteria, though they may influence different bacterial populations. Variety in your exercise routine may promote greater microbiome diversity. Even light activity like walking provides meaningful benefits compared to being sedentary.
Antibiotic Use and Medication Effects
Antibiotics kill both harmful pathogens and beneficial bacteria. A single course of broad-spectrum antibiotics can reduce bacterial diversity for months or years. Some species may never fully recover. While antibiotics save lives when truly needed, overuse causes lasting microbiome damage.
Take antibiotics only when medically necessary for bacterial infections. Viral illnesses do not respond to antibiotics. Discuss narrow-spectrum options with your doctor when possible, as these target specific bacteria while sparing beneficial species.
During and after antibiotic treatment, emphasize fermented foods and diverse plant foods to help restore beneficial bacteria. Some evidence suggests that specific probiotic strains can reduce antibiotic-associated diarrhea. Continue gut-supportive nutrition for several months after completing antibiotics.
Many common medications beyond antibiotics affect gut bacteria. Proton pump inhibitors for acid reflux, metformin for diabetes, and NSAIDs for pain all alter the microbiome. Discuss these effects with your healthcare provider and explore alternatives when appropriate.
Hydration and Digestive Function
Adequate water intake supports the mucosal lining of the intestines where beneficial bacteria reside. Dehydration can alter gut bacteria composition and impair the protective mucus layer. Water also helps fiber move through your digestive system and prevents constipation.
The gut bacteria themselves influence hydration status by affecting how your colon absorbs water. An imbalanced microbiome can contribute to chronic constipation or diarrhea through disrupted water regulation. Proper hydration supports beneficial bacteria that maintain normal bowel function.
Aim for eight to ten glasses of water daily, adjusting for activity level and climate. Herbal teas and naturally flavored water count toward hydration goals. Limiting caffeine and alcohol prevents dehydration that can stress gut bacteria.
Get Expert Guidance on Optimizing Your Gut Health
Understanding gut health principles is just the beginning. Implementing an effective strategy that combines the right foods, supplements, and lifestyle changes requires expert guidance. This free video presentation reveals the exact system used by thousands to restore their gut microbiome and overcome chronic digestive issues. Discover how to address the root causes of gut dysfunction, not just the symptoms.
Implementing Your Gut Health Diet: Practical Strategies
Transitioning to a gut health diet requires planning and gradual changes. Sudden dramatic shifts can cause temporary digestive discomfort as your bacterial populations adjust. A strategic approach allows your microbiome to adapt while building sustainable habits.
Success comes from focusing on adding beneficial foods rather than only eliminating harmful ones. This positive framework makes dietary changes feel less restrictive. Small consistent improvements compound over time into significant microbiome transformation.
Creating a Gut-Healthy Meal Plan
Start each day with fiber-rich foods to feed morning bacterial activity. Overnight oats with berries, nuts, and ground flaxseed provide diverse fibers and polyphenols. Greek yogurt with fruit and a small amount of granola offers probiotics with prebiotic fuel.
Build lunch and dinner around vegetables, covering half your plate with colorful plant foods. Include a variety of vegetables throughout the week rather than eating the same ones daily. Rotate between leafy greens, cruciferous vegetables, root vegetables, and colorful options like peppers and tomatoes.
Add a serving of fermented food to at least one meal daily. Kimchi or sauerkraut pairs well with lunch or dinner. Kefir works as a breakfast drink or smoothie base. Miso can flavor soups and dressings.
Include legumes four to five times per week for prebiotic fiber and plant protein. Lentil soup, chickpea curry, black bean tacos, and hummus with vegetables provide variety. Preparing a large batch of beans on weekends simplifies weekday meals.
Sample Day of Gut-Healthy Eating
Breakfast: Steel-cut oats cooked with cinnamon, topped with blueberries, walnuts, and a dollop of plain kefir.
Morning Snack: Apple slices with almond butter and a small handful of almonds.
Lunch: Large salad with mixed greens, chickpeas, cucumber, tomatoes, shredded carrots, sauerkraut, olive oil, and lemon dressing. Whole grain crackers on the side.
Afternoon Snack: Carrot and celery sticks with hummus, green tea.
Dinner: Baked salmon with roasted Brussels sprouts and sweet potato. Side of kimchi. Fresh berries for dessert.
Evening: Small piece of dark chocolate and herbal tea.
Meal Prep Strategies
Dedicate two hours each week to prepare gut-healthy components. Cook a large pot of beans or lentils. Chop vegetables for quick salads and snacks. Prepare a batch of whole grains like quinoa or brown rice. Make a jar of sauerkraut or ferment vegetables. Having these elements ready makes assembling gut-healthy meals effortless throughout the week.
Gradual Transition Techniques
Add one new gut-healthy food each week rather than overhauling your entire diet overnight. This week, introduce chia seeds to your breakfast. Next week, try kimchi with lunch. The following week, swap white rice for quinoa. Slow incorporation allows your taste preferences and digestive system to adapt.
Increase fiber intake gradually to prevent bloating and gas. If you currently eat minimal fiber, add just five grams daily for one week. The next week, add another five grams. Continue this pattern until reaching twenty-five to thirty-eight grams daily. Your bacteria need time to adjust to higher fiber levels.
Start fermented foods with small portions. Begin with one tablespoon of sauerkraut or kimchi daily. After one week, increase to two tablespoons if you tolerate it well. Work up to a quarter cup or more over several weeks. Initial gas or bloating typically subsides as beneficial bacteria establish themselves.
Replace one problematic food at a time rather than eliminating everything simultaneously. This month, replace soda with water or unsweetened tea. Next month, swap white bread for whole grain. Focus on sustainable substitutions that you can maintain long-term.
Overcoming Common Challenges
Digestive symptoms during transition are normal and usually temporary. Bloating, gas, or changes in bowel movements occur as bacterial populations shift. These symptoms typically improve within two to four weeks. If problems persist or worsen, consult a healthcare provider.
Budget concerns about buying fresh produce and fermented foods are valid. Focus on affordable gut-healthy options like dried beans, frozen vegetables, cabbage for homemade sauerkraut, and oats. Buying seasonal produce and shopping sales reduces costs significantly.
Time constraints make convenience important. Batch cooking on weekends provides ready meals. Keeping frozen vegetables, canned beans, and quick-cooking grains like quinoa on hand enables fast gut-healthy meals. Simple preparations work as well as elaborate recipes.
Social situations and dining out present challenges. Research restaurant menus ahead of time to identify gut-friendly options. Most restaurants can accommodate requests for extra vegetables and simple preparations. Bringing a fermented food side dish to gatherings ensures you have gut-healthy options.

Tracking Your Progress
Keep a food and symptom journal for the first month of dietary changes. Record what you eat, portion sizes, and any digestive symptoms. Note energy levels, mood, and sleep quality. Patterns emerge that help you identify which foods work best for your unique microbiome.
Take photos before starting your gut health diet journey. Document physical changes, but remember that gut health improvements often manifest in ways beyond appearance. Better digestion, increased energy, improved mood, and reduced inflammation matter more than aesthetic changes.
Expect gradual improvements rather than overnight transformation. Some people notice changes within days, while others require weeks or months. Bacterial populations shift slowly. Consistent effort over three to six months typically produces significant, lasting results.
Consider working with a registered dietitian specializing in gut health if you have complex digestive issues. Professional guidance helps navigate conditions like inflammatory bowel disease, irritable bowel syndrome, or food intolerances. Personalized recommendations address your specific situation.
Long-Term Sustainability
The goal is permanent dietary pattern change, not a temporary diet. Focus on foods you genuinely enjoy rather than forcing yourself to eat things you dislike. Experiment with different preparations and recipes to find versions that appeal to you.
Follow the eighty-twenty rule for sustainable results. Eat gut-healthy foods eighty percent of the time, allowing flexibility for the remaining twenty percent. Perfect adherence is unnecessary and often counterproductive. Consistency matters more than perfection.
Adapt your gut health diet to your cultural background and food preferences. Every cuisine includes gut-healthy options. Indian cuisine offers lentils and yogurt. Asian traditions include fermented vegetables and miso. Mediterranean diets emphasize olive oil and vegetables. Find the intersection of gut health and your food heritage.
Regularly reassess and adjust your approach as your gut health improves. Foods that initially caused symptoms may become tolerable as your microbiome strengthens. Continue expanding the diversity of plant foods you consume. Your microbiome thrives on variety and new challenges.
Gut Health and Common Digestive Conditions
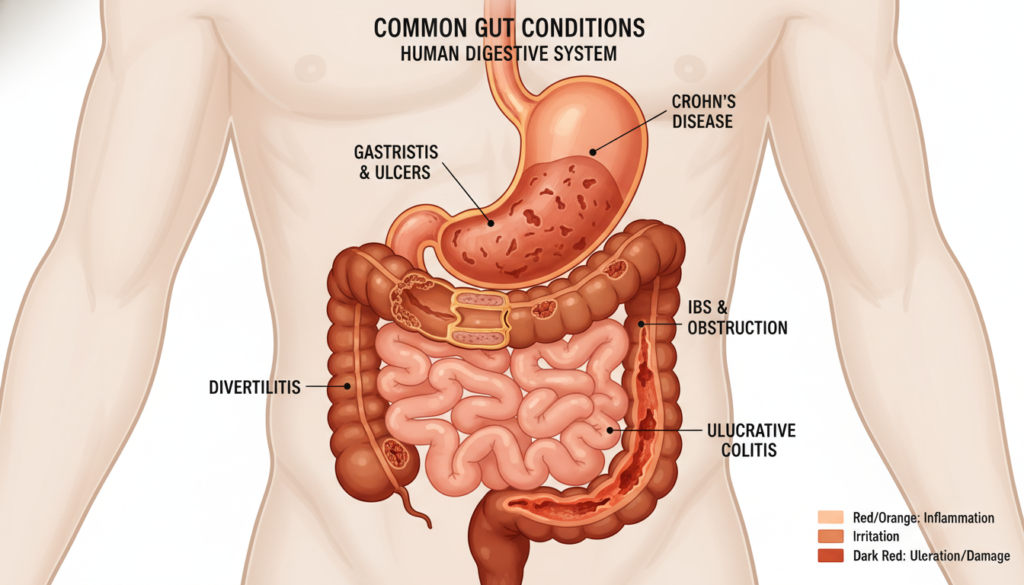
Specific digestive conditions benefit from targeted dietary approaches that address underlying microbiome dysfunction. Understanding how diet influences these conditions empowers you to manage symptoms and potentially achieve remission. While these strategies support gut health, they complement rather than replace medical treatment.
Each condition involves unique microbial imbalances and inflammatory patterns. Personalized dietary modifications based on individual symptoms and responses produce better outcomes than generic approaches. Working with healthcare providers ensures safe, effective treatment.
Inflammatory Bowel Disease Management
Inflammatory bowel disease includes Crohn’s disease and ulcerative colitis. These autoimmune conditions involve chronic intestinal inflammation and altered gut bacteria. Diet cannot cure inflammatory bowel disease, but specific foods can reduce inflammation and support remission.
During active flares, low-residue diets with easily digestible foods reduce bowel irritation. Well-cooked vegetables without skins, white rice, lean proteins, and smooth nut butters provide nutrition without aggravating inflammation. Avoid raw vegetables, whole grains, and high-fiber foods during acute symptoms.
The specific carbohydrate diet eliminates complex carbohydrates and processed foods while emphasizing vegetables, fruits, nuts, and animal proteins. Some inflammatory bowel disease patients achieve remission following this approach. The diet requires strict adherence and medical supervision.
Omega-3 fatty acids from fish oil demonstrate anti-inflammatory properties beneficial for inflammatory bowel disease. Consuming fatty fish like salmon, sardines, and mackerel two to three times weekly provides these fats. Supplementation may help some patients but should be discussed with doctors.
Certain probiotic strains show promise for maintaining remission in ulcerative colitis. VSL3, a high-potency probiotic mixture, has research supporting its use. However, probiotics during active Crohn’s disease flares may worsen symptoms in some individuals.
Irritable Bowel Syndrome Relief
Irritable bowel syndrome causes abdominal pain, bloating, and altered bowel habits without visible intestinal damage. Gut bacteria imbalances and increased intestinal sensitivity contribute to symptoms. The low FODMAP diet helps identify trigger foods for many irritable bowel syndrome patients.
FODMAPs are fermentable carbohydrates that bacteria rapidly ferment, producing gas and drawing water into the intestine. Common high-FODMAP foods include wheat, onions, garlic, certain fruits, and legumes. Temporarily eliminating these foods, then systematically reintroducing them, identifies personal triggers.
The low FODMAP diet should be temporary, lasting two to six weeks during elimination phase. Working with a dietitian ensures nutritional adequacy and proper reintroduction. Many people can eventually tolerate small amounts of previously problematic foods.
Peppermint oil capsules reduce irritable bowel syndrome symptoms in many patients. The oil relaxes intestinal muscles and reduces pain. Enteric-coated versions prevent heartburn and deliver the oil to the intestines.
Stress management particularly benefits irritable bowel syndrome given the strong gut-brain connection. Cognitive behavioral therapy, hypnotherapy, and mindfulness meditation all show effectiveness in clinical trials. These approaches address the neurological component of symptom generation.
Small Intestinal Bacterial Overgrowth
Small intestinal bacterial overgrowth occurs when excessive bacteria colonize the small intestine, where bacterial populations should remain low. These bacteria ferment food prematurely, causing bloating, pain, diarrhea, and nutrient malabsorption. Breath testing helps diagnose this condition.
Treatment typically involves antibiotics to reduce bacterial overgrowth followed by dietary changes to prevent recurrence. The specific protocol depends on which gases bacteria produce. Rifaximin is commonly prescribed due to its targeted action in the intestines.
After antibiotic treatment, a modified low-FODMAP diet prevents bacterial regrowth while the intestinal environment normalizes. Limiting fermentable carbohydrates starves excess bacteria. Gradually reintroducing diverse plant foods follows initial bacterial reduction.
Addressing underlying causes prevents small intestinal bacterial overgrowth recurrence. Conditions like low stomach acid, slow intestinal motility, and anatomical abnormalities contribute to bacterial overgrowth. Managing these root causes provides lasting relief.
Prokinetic agents that improve intestinal motility help prevent bacterial accumulation. Natural options include ginger and certain herbal preparations. Prescription medications may be necessary for some patients with significantly impaired motility.
| Condition | Dietary Approach | Key Foods to Emphasize | Foods to Limit |
| Inflammatory Bowel Disease (Active) | Low-residue, anti-inflammatory | Well-cooked vegetables, lean proteins, omega-3 fish, smooth nut butters | Raw vegetables, whole grains, high-fiber foods, dairy (if lactose intolerant) |
| Inflammatory Bowel Disease (Remission) | Mediterranean-style, diverse plants | Fatty fish, olive oil, cooked vegetables, fermented foods, fruits | Processed foods, excess red meat, alcohol, refined sugars |
| Irritable Bowel Syndrome | Low FODMAP (temporary), personalized | Low-FODMAP fruits/vegetables, rice, quinoa, lactose-free dairy, lean proteins | High-FODMAP foods (wheat, onions, garlic, certain fruits, legumes during elimination) |
| Small Intestinal Bacterial Overgrowth | Modified low-FODMAP, low-fermentation | Easily digestible proteins, cooked low-FODMAP vegetables, white rice | High-FODMAP foods, excess fiber during treatment, simple sugars |
| Diverticulitis (Acute) | Low-fiber, clear liquids initially | Broths, well-cooked low-fiber foods, lean proteins, gradually progress | High-fiber foods, nuts, seeds, raw vegetables during acute phase |
| Diverticulitis (Prevention) | High-fiber, diverse plants | Whole grains, vegetables, fruits, legumes, adequate hydration | Red meat, processed foods, low-fiber refined grains |
Addressing Chronic Constipation
Chronic constipation often involves inadequate fiber intake, poor hydration, and imbalanced gut bacteria. Gradually increasing fiber while ensuring adequate water intake typically improves symptoms. Aim for twenty-five to thirty-eight grams of fiber daily from diverse sources.
Soluble fiber from oats, chia seeds, and psyllium husk draws water into stool, softening it. Insoluble fiber from vegetables and wheat bran adds bulk and speeds transit time. Both types work together to promote regular bowel movements.
Prunes and prune juice contain sorbitol, a natural laxative, along with fiber. Eating five to six prunes daily effectively relieves constipation for many people. The combination of fiber and sorbitol provides gentle, natural relief.
Regular physical activity stimulates intestinal motility and improves constipation. Even short walks after meals encourage bowel movements. Establishing a consistent bathroom routine also helps by training your body’s natural reflexes.
Magnesium supplementation can relieve constipation by drawing water into the intestines. Start with a low dose and increase gradually to avoid diarrhea. Magnesium citrate works more effectively than other forms for this purpose.
Managing Diarrhea and Loose Stools
Chronic diarrhea has numerous potential causes including infections, inflammatory conditions, and food intolerances. Identifying and addressing the underlying cause proves essential. Persistent diarrhea requires medical evaluation to rule out serious conditions.
Soluble fiber paradoxically helps both constipation and diarrhea by regulating stool consistency. Psyllium husk, oat bran, and pectin from cooked apples absorb excess water in loose stools. These fibers also feed beneficial bacteria that improve gut barrier function.
Probiotic strains including Saccharomyces boulardii and specific Lactobacillus species reduce diarrhea duration and severity. These organisms compete with harmful bacteria and support intestinal barrier integrity. Quality matters significantly in probiotic effectiveness.
Avoiding common trigger foods helps identify dietary causes. Lactose, artificial sweeteners, caffeine, and high-fat foods commonly trigger diarrhea. Systematic elimination and reintroduction reveals personal sensitivities.
Bile acid malabsorption causes diarrhea in some people after gallbladder removal or with certain conditions. Specific supplements and medications can bind excess bile acids. Medical testing confirms this diagnosis.
Testing and Monitoring Your Gut Health
Various tests provide insights into your gut microbiome composition and digestive function. These assessments help identify specific imbalances and guide targeted interventions. Understanding what different tests reveal helps you make informed decisions about testing options.
Not everyone needs comprehensive gut testing. Clinical symptoms and response to dietary changes often provide sufficient guidance. However, people with persistent digestive issues or chronic health conditions may benefit from detailed analysis.
Comprehensive Stool Analysis
Comprehensive stool tests analyze bacterial diversity, specific bacterial species, yeast overgrowth, parasites, and markers of inflammation. These tests provide detailed snapshots of your gut ecosystem. Results identify beneficial bacteria deficiencies and potentially harmful organism overgrowth.
Many commercial companies offer at-home stool testing kits. Quality and accuracy vary significantly between providers. Look for labs that use DNA sequencing technology rather than culture-based methods for more comprehensive bacterial identification.
Test results typically include bacterial diversity scores, ratios of beneficial to harmful organisms, and specific species populations. Some tests also measure digestive enzymes, inflammatory markers, and immune function indicators. Interpreting these results often requires professional guidance.
Stool tests represent a single point in time and can vary based on recent diet, medications, and stress levels. Retesting after implementing changes tracks progress and guides ongoing adjustments. Most practitioners recommend waiting at least three months between tests.
Breath Testing for Bacterial Overgrowth
Hydrogen and methane breath tests detect small intestinal bacterial overgrowth and carbohydrate malabsorption. After consuming a sugar solution, you breathe into collection tubes at timed intervals. Elevated gases indicate bacterial fermentation in the small intestine.
These tests help diagnose small intestinal bacterial overgrowth and identify whether hydrogen-producing or methane-producing bacteria predominate. This information guides treatment selection, as different antibiotics target different bacterial types. Proper test preparation ensures accurate results.
Breath tests also identify lactose intolerance and fructose malabsorption. Gas production after consuming these specific sugars confirms digestive enzyme deficiencies or absorption problems. These diagnoses inform dietary modifications.
False negatives can occur if patients recently used antibiotics or certain supplements. Following preparation instructions precisely improves test accuracy. Working with knowledgeable practitioners ensures proper test selection and interpretation.
Functional Medicine Testing
Organic acid testing analyzes urine metabolites produced by bacteria, yeast, and human cells. This test provides indirect information about gut bacteria balance, yeast overgrowth, and neurotransmitter metabolism. Results can identify bacterial byproducts associated with specific conditions.
Intestinal permeability testing measures how well your intestinal barrier functions. The lactulose-mannitol test involves drinking a solution containing these sugars and measuring their urinary excretion. High levels indicate increased intestinal permeability or “leaky gut.”
Zonulin is a protein that regulates intestinal permeability. Blood tests measuring zonulin levels indicate barrier function. Elevated zonulin suggests compromised gut barrier integrity that may benefit from targeted healing protocols.
These specialized tests cost more than standard medical tests and may not be covered by insurance. Consider whether the information gained will meaningfully change your treatment approach. Sometimes empirical dietary trials prove more practical and cost-effective.
Working with Test Results
Test results provide data points but require expert interpretation within your full clinical context. A functional medicine practitioner, integrative gastroenterologist, or specialized dietitian can translate findings into actionable protocols. Avoid making drastic changes based solely on test results without professional guidance. Symptoms, medical history, and individual response to interventions matter as much as laboratory values.
Self-Assessment and Symptom Tracking
Detailed symptom journals often reveal patterns that laboratory tests miss. Record bowel movement frequency and consistency, energy levels, mood, sleep quality, skin condition, and any digestive discomfort. Note specific foods eaten and their timing relative to symptoms.
The Bristol Stool Chart provides a standardized way to assess stool consistency. Types 3 and 4 indicate healthy transit time and hydration. Consistent type 1 or 2 suggests constipation. Type 6 or 7 indicates diarrhea. Tracking trends helps evaluate intervention effectiveness.
Energy fluctuations throughout the day can relate to blood sugar regulation influenced by gut bacteria. Noting energy patterns alongside meals reveals connections between specific foods and how you feel. Stable energy suggests good metabolic health.
Skin conditions like acne, eczema, and rosacea often improve with gut healing. Photographing skin condition monthly provides objective evidence of progress. Many gut health improvements manifest in skin quality before digestive symptoms fully resolve.
Mental clarity, mood stability, and stress resilience all connect to gut health through the gut-brain axis. Rating these factors weekly on a simple scale helps track less tangible improvements. Many people notice mental and emotional benefits before physical changes.
Supplements That Support Gut Health

While whole foods should form the foundation of gut health, targeted supplements can accelerate healing and address specific deficiencies. Quality varies dramatically between products. Understanding which supplements provide genuine benefits helps you make informed purchasing decisions.
Supplements complement but never replace a healthy gut health diet. No pill can compensate for poor dietary choices. Use supplements strategically to address identified needs while continuing to emphasize food-based nutrition.
Probiotic Supplements
Probiotic supplements contain live beneficial bacteria that can colonize your gut. Different strains provide different benefits. Lactobacillus and Bifidobacterium species are most commonly used and well-researched. Multi-strain formulas typically offer broader benefits than single-strain products.
Colony-forming units indicate the number of viable bacteria. Look for products with at least 10 billion CFUs per dose. Higher numbers do not necessarily mean better results. Strain selection matters more than total bacterial count.
Shelf-stable probiotics use special technology to keep bacteria viable without refrigeration. Refrigerated products may contain more fragile strains. Both can be effective when properly manufactured and stored. Check expiration dates and storage requirements.
Take probiotics consistently for at least four weeks to assess effectiveness. Some people notice improvements within days, while others require months. If a particular product causes digestive upset, try a different strain combination. Individual responses vary significantly.
Timing recommendations vary by strain. Some probiotics work best on an empty stomach, while others prefer food. Follow manufacturer instructions. Taking probiotics at the same time daily helps establish consistent dosing habits.
Prebiotic Supplements
Prebiotics feed beneficial bacteria already in your gut. Inulin, fructooligosaccharides, and galactooligosaccharides are common prebiotic fibers. These supplements increase populations of beneficial bacteria while providing fiber your diet may lack.
Start prebiotic supplements with small doses to prevent gas and bloating. Your bacteria need time to adapt to increased fermentable fiber. Gradually increase the dose over several weeks as tolerance improves.
Whole food sources of prebiotics like chicory root, Jerusalem artichoke, and green bananas provide additional nutrients along with prebiotic fiber. Supplements offer concentrated doses that can be helpful when whole food intake is insufficient.
Combining prebiotics with probiotics, called synbiotics, may enhance effectiveness. The prebiotics feed the probiotic bacteria, helping them establish themselves. Some products package these together in synbiotic formulas.
Digestive Enzymes
Digestive enzyme supplements break down proteins, fats, and carbohydrates when your body produces insufficient natural enzymes. People with pancreatic insufficiency, inflammatory bowel disease, or aging-related enzyme decline may benefit from supplementation.
Broad-spectrum enzyme formulas contain protease for protein, lipase for fats, and amylase for carbohydrates. Some products add lactase for lactose digestion or alpha-galactosidase for breaking down beans and cruciferous vegetables.
Take digestive enzymes at the beginning of meals for optimal effectiveness. The enzymes work alongside your natural digestive processes. Consistency matters more than occasional use.
Not everyone needs digestive enzymes. If you digest food well and have no symptoms, adding enzymes provides no benefit. Consider enzymes if you experience bloating, gas, or undigested food in stool despite dietary improvements.
L-Glutamine for Gut Barrier Support
L-glutamine is an amino acid that intestinal cells use for energy and repair. Supplementation may help heal intestinal permeability or “leaky gut.” Athletes, people with inflammatory bowel disease, and those recovering from intestinal infections may benefit.
Typical doses range from five to fifteen grams daily, divided into two or three doses. Higher doses may cause digestive upset in some people. Start with a lower dose and increase gradually.
Glutamine powder mixes easily into water or smoothies. The powder form typically costs less than capsules and allows flexible dosing. Some people prefer capsules for convenience despite higher cost.
Research on glutamine for gut healing shows mixed results. Some studies demonstrate clear benefits for intestinal barrier function, while others show minimal effects. Individual response varies. Trial periods of two to three months allow adequate assessment.
Omega-3 Fatty Acids
Fish oil supplements provide EPA and DHA omega-3 fatty acids that reduce intestinal inflammation. These fats also influence gut bacteria composition, promoting species associated with lower inflammation. Most people benefit from omega-3 supplementation given inadequate dietary intake.
Quality varies significantly between fish oil products. Look for third-party testing for purity and concentration. Certifications from organizations like IFOS indicate products meet quality standards and contain minimal contaminants.
Typical doses for anti-inflammatory effects range from one to three grams of combined EPA and DHA daily. Higher doses may thin blood, so discuss supplementation with your doctor if you take blood-thinning medications.
Algae-based omega-3 supplements provide EPA and DHA from plant sources suitable for vegetarians and vegans. These products offer similar benefits to fish oil without sustainability or contamination concerns associated with fish.
Learn the Complete Gut Restoration System
Choosing the right supplements can feel overwhelming with countless products making bold claims. This comprehensive video presentation reveals exactly which supplements actually work based on scientific research and clinical results. Discover the precise combination of diet, supplementation, and lifestyle strategies that address gut dysfunction at its root. Thousands have used this systematic approach to transform their digestive health and overall wellbeing.
Zinc Carnosine
Zinc carnosine supports the integrity of the stomach and intestinal lining. This supplement may help heal stomach ulcers, reduce inflammation, and strengthen the gut barrier. People with inflammatory bowel disease or chronic NSAID use may find particular benefit.
Standard dosing uses 75 to 150 milligrams of zinc carnosine taken between meals. The chelated form provides better absorption and tolerability than standard zinc supplements. Continue for at least eight weeks to assess effectiveness.
Zinc carnosine works differently than regular zinc supplements. The carnosine component helps deliver zinc directly to damaged intestinal tissue. This targeted delivery enhances healing effects compared to standard zinc forms.
Curcumin for Inflammation
Curcumin, the active compound in turmeric, demonstrates powerful anti-inflammatory effects in the digestive tract. Research shows benefits for inflammatory bowel disease, irritable bowel syndrome, and general gut inflammation. Poor absorption limits effectiveness without enhancement.
Look for curcumin supplements with bioavailability enhancers like black pepper extract (piperine), phospholipids, or special formulations. These technologies increase absorption twenty to one hundred times compared to standard curcumin.
Effective doses typically range from 500 to 2000 milligrams daily, depending on formulation and condition severity. Divide doses throughout the day for sustained anti-inflammatory effects. Consistent daily use produces better results than occasional supplementation.
Choosing Quality Supplements
Third-party testing certifications from organizations like NSF International, USP, or ConsumerLab indicate products meet quality standards. These certifications verify that supplements contain stated ingredients in listed amounts without harmful contaminants.
Manufacturing practices matter significantly. Look for products made in GMP-certified facilities that follow good manufacturing practices. This ensures consistent quality and safety standards.
Price often reflects quality in supplements. Extremely cheap products may use inferior ingredients or inadequate doses. However, expensive does not always mean better. Research specific brands and read independent reviews before purchasing.
Consult healthcare providers before starting new supplements, especially if you take medications or have medical conditions. Some supplements interact with medications or may not be appropriate for certain conditions. Professional guidance ensures safe, effective supplementation.
Gut Health Across Different Life Stages
Gut health needs change throughout life from infancy through older age. Understanding these stage-specific considerations helps optimize microbiome health at every age. Dietary strategies that work for adults may not suit infants or elderly individuals.
Early life experiences particularly impact long-term gut health. However, the microbiome remains adaptable throughout life. Positive changes at any age can improve bacterial diversity and overall health outcomes.
Infant Gut Development
Infants acquire their initial gut bacteria during birth and through early feeding. Vaginal delivery exposes babies to maternal bacteria that seed the infant microbiome. Cesarean-born babies have different initial bacterial colonization that gradually normalizes over months.
Breastfeeding provides unique oligosaccharides that feed beneficial Bifidobacteria species. These bacteria dominate healthy infant guts and protect against pathogens. Breast milk also contains antibodies and immune factors that support gut barrier development.
Formula-fed infants develop different microbiome patterns than breastfed babies. Modern formulas include prebiotics to support beneficial bacteria growth. However, composition still differs from breastfed infant microbiomes.
Introduction of solid foods around six months dramatically shifts infant gut bacteria. Offering diverse fruits, vegetables, and whole foods early encourages bacterial diversity. Avoiding ultra-processed foods and added sugars during this critical window supports optimal development.
Antibiotic exposure during infancy can disrupt microbiome development with lasting effects. Use antibiotics only when medically necessary. Probiotic supplementation during and after infant antibiotic treatment may reduce negative impacts.
Childhood Nutrition and Gut Health
Children who eat diverse plant foods develop greater bacterial diversity than those with limited vegetable intake. Establishing healthy eating patterns early creates microbiome advantages that persist into adulthood. Childhood represents a critical window for microbiome education.
Excessive sugar and processed food consumption during childhood promotes obesity-associated bacteria. These bacterial patterns can persist even when diet improves later. Prevention through early healthy habits proves easier than reversing established patterns.
Exposure to pets, outdoor play, and diverse environments supports bacterial diversity in children. Overly sterile environments may limit beneficial bacterial exposure. Balance between cleanliness and appropriate microbial contact supports immune development.
Food allergies and eczema in children often relate to gut health and barrier function. Early introduction of diverse foods, including common allergens, may reduce allergy development. Current guidelines recommend introducing peanuts, eggs, and other allergens during infancy rather than delaying exposure.

Gut Health During Pregnancy
Pregnancy naturally alters maternal gut bacteria to support fetal development and prepare for lactation. Bacterial changes during pregnancy affect nutrient absorption, immune function, and metabolism. Supporting healthy bacteria during pregnancy benefits both mother and baby.
Probiotic supplementation during pregnancy may reduce gestational diabetes risk and support healthy weight gain. Certain strains also decrease infant eczema and allergy risk. Choose pregnancy-safe probiotic strains and consult healthcare providers.
Maintaining adequate fiber intake during pregnancy prevents constipation and supports beneficial bacteria. Most pregnant women need slightly more fiber than usual. Focus on fruits, vegetables, and whole grains unless specific conditions require modification.
Maternal gut bacteria influence infant immune system development before birth through immune signaling molecules. A healthy maternal microbiome programs the infant immune system appropriately. This highlights the importance of maternal gut health during pregnancy.
Aging and Microbiome Changes
Gut bacteria diversity typically declines with age. Elderly individuals often show reduced beneficial bacteria and increased pro-inflammatory species. This shift contributes to inflammaging, the chronic low-grade inflammation associated with aging.
Dietary diversity becomes even more important with age to maintain bacterial populations. Older adults often eat fewer different foods, which reduces bacterial diversity. Consciously varying food choices helps preserve microbiome health.
Reduced stomach acid production with age affects bacterial populations and increases infection risk. Probiotic supplements may help compensate for age-related changes. Fermented foods provide both probiotics and enhanced nutrient absorption.
Medications common in older age including proton pump inhibitors, antibiotics, and NSAIDs all disrupt gut bacteria. Minimizing unnecessary medications and supporting gut health through diet becomes increasingly important.
Physical activity helps maintain gut bacteria diversity in older adults. Regular exercise prevents the bacterial decline typically seen with aging. Even moderate activity like walking provides meaningful benefits.
Menopause and Gut Health
Hormonal changes during menopause affect gut bacteria composition. The microbiome influences how the body metabolizes estrogen. An unhealthy microbiome may worsen menopausal symptoms including weight gain and mood changes.
Phytoestrogens from soy, flaxseeds, and legumes require specific gut bacteria for activation. These bacteria convert plant compounds into forms that bind estrogen receptors. Supporting these bacteria may help manage menopausal symptoms.
Weight gain during menopause relates partly to shifts in gut bacteria metabolism. Maintaining bacterial diversity through diet helps regulate weight. Exercise combined with gut-healthy nutrition produces better results than diet alone.
Bone health during and after menopause depends partly on gut bacteria that produce vitamin K and regulate calcium absorption. Supporting these bacteria through fermented foods and diverse plants protects bone density.
The Future of Gut Health Research and Personalized Nutrition
Gut health research represents one of the fastest-growing areas in medical science. New discoveries emerge regularly about how gut bacteria influence health and disease. Understanding these developments helps anticipate future treatment options and dietary recommendations.
The field moves toward increasingly personalized nutrition based on individual microbiome composition. What works for one person may not work for another due to unique bacterial populations. Future recommendations will likely account for this individual variation.
Emerging Research Areas
Scientists now investigate gut bacteria’s role in conditions previously not connected to digestion. Research explores connections between the microbiome and autism, Parkinson’s disease, multiple sclerosis, and various cancers. While connections exist, causal relationships require further study.
The gut-skin axis reveals how intestinal bacteria influence skin conditions including acne, psoriasis, and premature aging. Specific bacterial metabolites affect skin through systemic circulation. This research may lead to novel treatments for chronic skin conditions.
Microbiome-based diagnostics may eventually predict disease risk and treatment responses. Bacterial patterns could indicate who will develop specific conditions years before symptoms appear. This predictive capability would enable preventive interventions.
Engineered probiotics represent an exciting frontier. Scientists modify bacteria to produce specific therapeutic compounds or perform particular functions. These designer probiotics might treat conditions from inflammation to cancer.
Personalized Nutrition Based on Microbiome
Current dietary recommendations provide general guidelines suitable for most people. Future nutrition advice may specify exact foods based on individual microbiome analysis. Some companies already offer such services, though scientific validation remains limited.
Glycemic response to foods varies significantly between individuals based partly on gut bacteria. The same food causes different blood sugar responses in different people. Personalized nutrition accounts for these individual differences.
Nutrient absorption efficiency depends on bacterial populations. Some people extract more calories from food than others eating identical diets. Understanding personal bacterial capabilities could optimize nutrition for individual goals.
Food sensitivity and intolerance patterns relate to microbiome composition. Testing might eventually predict which foods an individual will tolerate based on their bacteria. This would eliminate trial-and-error elimination diets.
Current Limitations
While personalized microbiome testing shows promise, current science cannot yet provide highly specific dietary recommendations for most people. Bacterial populations fluctuate, and we still do not fully understand which patterns indicate optimal health versus disease risk. General principles like eating diverse plants, fermented foods, and avoiding processed ingredients remain the most evidence-based approach for now.
Fecal Microbiota Transplantation
Fecal microbiota transplantation involves transferring stool from healthy donors to recipients with compromised microbiomes. This treatment shows remarkable effectiveness for recurrent Clostridioides difficile infection, curing over ninety percent of cases.
Researchers investigate fecal transplantation for inflammatory bowel disease, irritable bowel syndrome, obesity, and metabolic conditions. Results vary, with some studies showing benefits and others finding limited effects. Standardization and donor selection remain challenges.
Safety concerns include the potential transfer of unknown pathogens or disease-promoting bacteria. Rigorous donor screening reduces but does not eliminate risks. Long-term effects of introducing someone else’s microbiome remain unknown.
Synthetic stool alternatives containing defined bacterial mixtures may eventually replace human donor stool. These standardized products would offer consistent composition and eliminate infection risks. Several companies develop such therapeutics.
Practical Applications Today
While future developments promise exciting possibilities, proven strategies exist now for improving gut health. Emphasizing diverse plant foods, fermented products, adequate fiber, and limited processed foods works for nearly everyone regardless of individual microbiome composition.
Basic lifestyle factors including sleep, stress management, exercise, and medication stewardship dramatically impact gut health. These foundational elements require no expensive testing or specialized protocols. Implementation delivers real benefits today.
Rather than waiting for perfect personalized recommendations, start with well-established principles. Monitor your individual response and adjust accordingly. Your symptoms, energy, and overall wellbeing provide valuable feedback about what works for your unique microbiome.
Stay informed about research developments without chasing every new trend. Fundamental gut health principles remain constant even as specific details evolve. Focus on sustainable dietary patterns rather than short-term interventions.
Taking Control of Your Gut Health Journey

Your gut microbiome represents a powerful determinant of overall health that you can influence daily through food choices. Every meal presents an opportunity to feed beneficial bacteria or harmful ones. The cumulative effect of these choices shapes your long-term health trajectory.
Implementing a gut health diet does not require perfection or expensive specialty products. Focus on adding more diverse plant foods, fermented options, and whole grains while reducing processed items. These fundamental changes produce meaningful results regardless of your starting point.
Progress unfolds gradually as bacterial populations shift over weeks and months. Initial digestive changes may feel uncomfortable as your microbiome adjusts. Persistence through this transition period leads to lasting improvements in digestion, immunity, energy, and overall wellbeing.
Individual responses to dietary changes vary based on your unique microbiome composition and health status. What works optimally for one person may need adjustment for another. Pay attention to your body’s signals and modify your approach accordingly.
Beyond diet, lifestyle factors including sleep quality, stress management, and physical activity significantly impact gut health. Address these elements alongside nutrition for comprehensive microbiome support. Small improvements across multiple areas create synergistic benefits.
The gut-brain connection means that improving gut health often enhances mental clarity, mood stability, and stress resilience. Many people notice psychological benefits before physical symptoms fully resolve. These mental health improvements provide additional motivation to maintain gut-healthy habits.
Working with healthcare professionals helps navigate complex digestive conditions and ensures safe, effective interventions. While general principles apply broadly, personalized guidance addresses individual circumstances. Professional support accelerates progress and prevents common pitfalls.
Sustainable change comes from gradual habit formation rather than dramatic overnight transformation. Focus on progress, not perfection. Each gut-healthy choice builds upon previous ones, creating momentum toward lasting change.
Your gut health journey is unique and ongoing. The microbiome remains adaptable throughout life, responding to dietary and lifestyle modifications at any age. Positive changes today create benefits that extend far into the future.
Ready to Transform Your Gut Health?
You now understand the critical role your gut microbiome plays in overall health and how diet shapes bacterial populations. The next step involves implementing a comprehensive, science-backed system that addresses all aspects of gut restoration. This free expert presentation reveals the exact protocol that combines optimal nutrition, targeted supplementation, and lifestyle strategies for lasting gut health transformation. Discover how to heal your digestive system from the inside out and reclaim the vibrant health you deserve.
The knowledge you have gained here provides the foundation for informed decisions about your gut health. Implementation transforms information into results. Begin with one or two changes this week, building gradually toward a comprehensive gut health diet.
Remember that your gut bacteria work for you when you provide what they need. Diverse plant foods, fermented options, adequate fiber, and minimal processed ingredients create the environment where beneficial bacteria thrive. These organisms, in turn, support every system in your body.
Your health journey deserves the same attention and care you give to other important aspects of life. Investing in gut health pays dividends across physical, mental, and emotional wellbeing. The path forward begins with your very next meal.