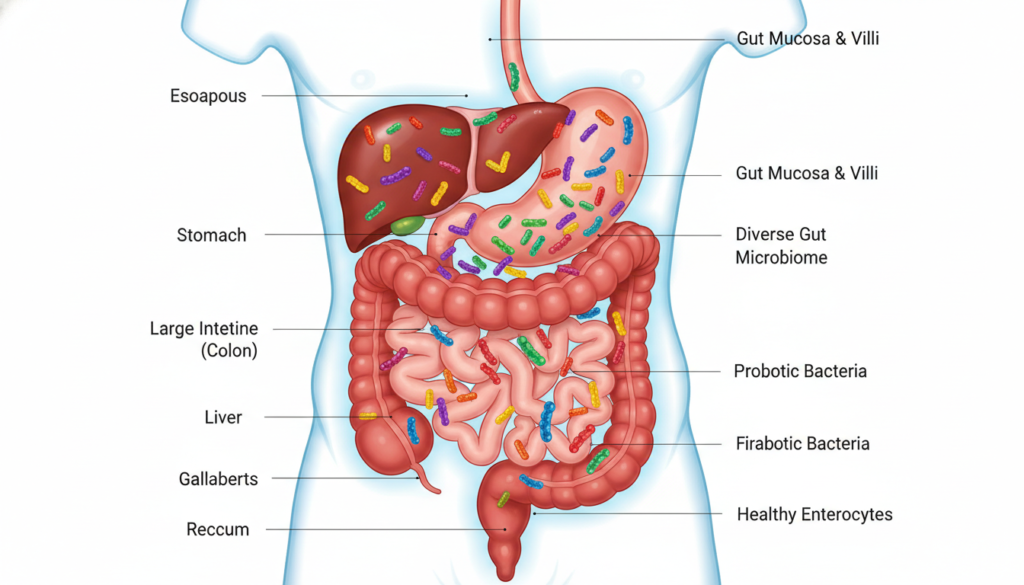
The health of your digestive system influences nearly every aspect of your wellbeing. Your gut microbiome contains trillions of microorganisms that regulate digestion, immunity, mood, and energy levels. When this delicate ecosystem falls out of balance, the consequences extend far beyond stomach discomfort.
This Website contains affiliate links. That means I may earn a small commission if you purchase through my links, at no extra cost to you.
Modern lifestyles create unprecedented challenges for maintaining optimal gut health. Processed foods, chronic stress, antibiotic use, and environmental toxins disrupt the bacterial balance your body needs. The result is a growing epidemic of digestive disorders and related health conditions.
Understanding how to improve gut health requires a comprehensive approach that addresses multiple factors simultaneously. This guide explores evidence-based strategies that restore balance to your gut microbiome and support long-term digestive wellness.
Understanding Your Gut Microbiome and Why It Matters
Your gut houses a complex community of bacteria, fungi, and other microorganisms collectively known as the gut microbiome. These microscopic inhabitants perform essential functions that keep your body operating properly. They break down nutrients, synthesize vitamins, train your immune system, and even produce neurotransmitters that affect your brain.
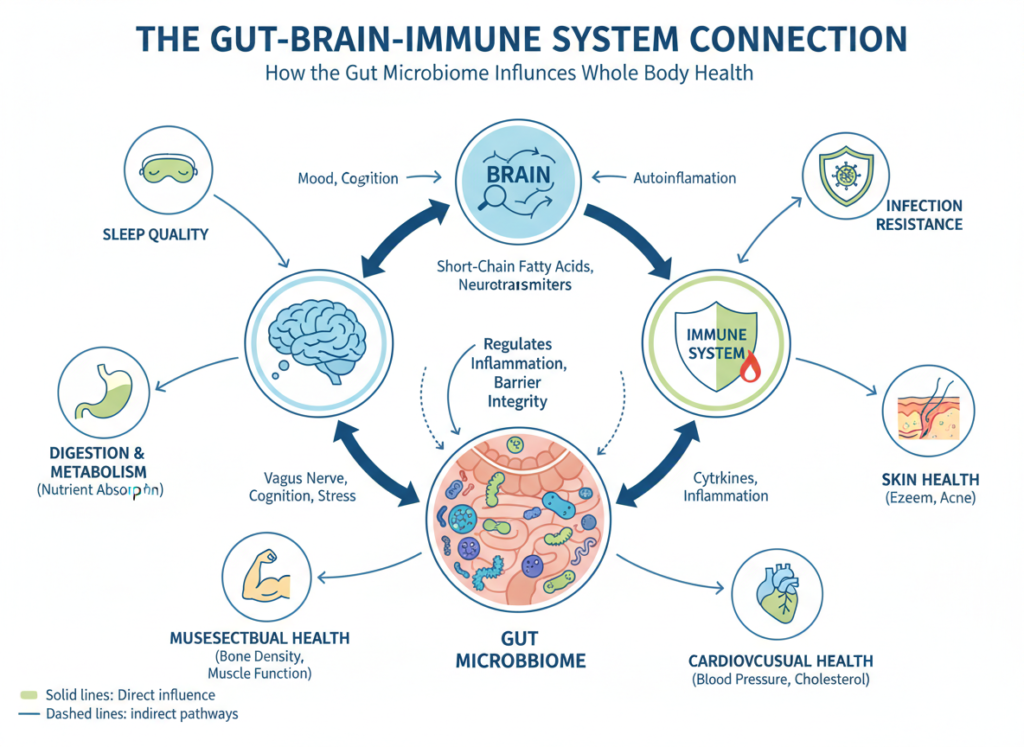
Research reveals that gut health impacts conditions ranging from obesity to depression. A diverse gut microbiome correlates with better overall health outcomes. Conversely, reduced bacterial diversity associates with inflammatory bowel disease, metabolic disorders, and autoimmune conditions.
The bacteria in your large intestine ferment fiber into short-chain fatty acids. These compounds provide energy to intestinal cells, reduce inflammation, and strengthen the gut barrier. Without sufficient beneficial bacteria, this protective process breaks down.
Your microbiome composition reflects your diet, lifestyle, medications, and environment. Every choice you make either supports or undermines these beneficial microorganisms. The good news is that targeted interventions can restore balance relatively quickly.
Recognizing Signs Your Gut Needs Attention
Your body sends clear signals when your gut microbiome needs support. Many people dismiss these symptoms as normal, but they indicate underlying imbalances that deserve attention. Recognizing these warning signs allows you to intervene before minor issues escalate.
Digestive Symptoms That Demand Action
Bloating represents one of the most common indicators of gut imbalance. When harmful bacteria overgrow, they produce excessive gas during digestion. This creates uncomfortable abdominal distension that worsens throughout the day.

Irregular bowel movements signal disrupted gut function. Constipation occurs when intestinal transit slows, often due to insufficient beneficial bacteria or low fiber intake. Diarrhea indicates irritation in the digestive tract or rapid transit that prevents proper nutrient absorption.
Persistent stomach pain or cramping suggests inflammation in the digestive system. The gut lining may be compromised, allowing irritants to trigger immune responses. This chronic inflammation damages intestinal tissue over time.
Systemic Symptoms Linked to Gut Health
Unexplained fatigue often stems from poor nutrient absorption. When your gut cannot properly extract vitamins and minerals from food, your energy levels plummet. Bacterial imbalances also affect how your body metabolizes nutrients.
Brain fog and difficulty concentrating connect directly to gut health through the gut-brain axis. Your intestinal bacteria produce neurotransmitters that influence cognitive function. Imbalanced gut microbiome disrupts these chemical signals.
Skin problems like acne, eczema, or rashes frequently originate in the gut. Inflammation in the digestive tract triggers systemic responses that manifest on your skin. Addressing gut health often resolves stubborn skin conditions.
Frequent infections indicate compromised immune function. Since 70% of your immune system resides in your gut, bacterial imbalances weaken your defenses. People with gut issues catch colds more often and recover more slowly.
Important: Experiencing multiple symptoms simultaneously strongly suggests gut microbiome disruption. The diversity of symptoms reflects how extensively your gut influences overall health.
Dietary Foundations for Gut Microbiome Health
The foods you consume directly shape your gut bacteria composition. Certain dietary patterns promote beneficial microorganisms while others encourage harmful species. Understanding these relationships empowers you to make choices that rebuild gut health.
Fiber: The Foundation of Gut Health
Dietary fiber serves as fuel for beneficial gut bacteria. These microorganisms ferment fiber into compounds that nourish your intestinal lining and reduce inflammation. Most people consume far less fiber than their gut microbiome needs.

Fruits and vegetables provide diverse fiber types that feed different bacterial strains. Aim for a wide range of plant foods to support microbiome diversity. Each type of produce contains unique compounds that benefit specific beneficial bacteria.
Legumes deliver exceptional fiber content alongside protein and resistant starch. Beans, lentils, and peas support robust bacterial populations in your large intestine. Regular consumption correlates with improved gut health markers.
Fermented Foods as Probiotic Sources
Fermented foods introduce live beneficial bacteria directly into your digestive tract. These natural probiotics colonize your gut and compete with harmful microorganisms. Traditional cultures have consumed fermented foods for thousands of years.
Yogurt with live active cultures provides easily accessible probiotics. Choose unsweetened varieties to avoid feeding harmful bacteria with excess sugar. Greek yogurt offers concentrated protein along with beneficial microorganisms.
Kimchi and sauerkraut contain diverse bacterial strains created through fermentation. These tangy vegetables also provide fiber and nutrients. Start with small portions and gradually increase as your system adapts.
Kefir delivers a wider range of probiotic strains than yogurt. This fermented beverage supports gut microbiome diversity more effectively than single-strain supplements. Look for traditionally fermented versions without added sugars.

Prebiotic Foods That Feed Good Bacteria
Prebiotics are specific fibers that selectively nourish beneficial gut bacteria. These compounds resist digestion in your stomach and reach your large intestine intact. There, they fuel the growth of health-promoting microorganisms.

Garlic contains inulin, a powerful prebiotic fiber. This aromatic ingredient supports specific beneficial bacteria while exhibiting antimicrobial properties against harmful strains. Both raw and cooked garlic provide gut health benefits.
Onions deliver fructooligosaccharides that feed Bifidobacteria species. These beneficial bacteria produce compounds that strengthen your gut barrier and reduce inflammation. Include onions regularly in your diet for consistent prebiotic support.
Asparagus provides inulin alongside vitamins and minerals. This vegetable supports beneficial bacteria growth while being relatively easy to digest. Lightly cooked asparagus offers optimal nutrient availability.
Critical Lifestyle Factors Affecting Gut Health
Your daily habits influence gut microbiome composition as profoundly as your diet. Sleep quality, stress levels, and physical activity all shape which bacteria thrive in your digestive system. Optimizing these lifestyle factors accelerates gut health improvement.
Sleep’s Profound Impact on Your Microbiome
Sleep deprivation disrupts gut bacteria balance and increases intestinal permeability. Research shows that people who sleep fewer than six hours nightly have less diverse gut microbiomes. Poor sleep also triggers inflammation throughout the digestive tract.

Your gut bacteria follow circadian rhythms just like the rest of your body. Irregular sleep schedules confuse these biological clocks and impair bacterial function. Consistent sleep timing supports optimal microbiome activity.
Aim for seven to nine hours of quality sleep each night. Create a dark, cool sleeping environment and establish a relaxing bedtime routine. These simple changes support both gut health and overall wellness.
Managing Stress to Protect Your Gut
Chronic stress directly damages gut health through the gut-brain axis. Stress hormones alter bacterial composition, increase intestinal permeability, and trigger inflammation. Many digestive symptoms worsen during stressful periods.

Stress reduction techniques provide measurable gut health benefits. Meditation, deep breathing exercises, and yoga all reduce stress hormones that harm your microbiome. Even brief daily practice makes a difference.
Regular breaks throughout your day prevent chronic stress accumulation. Step away from work, practice mindful breathing, or take short walks. These micro-interventions protect your gut from stress-related damage.
Social connections and meaningful relationships buffer against stress. People with strong social support show healthier gut microbiome profiles. Prioritize time with friends and family as part of your gut health strategy.
Exercise and Gut Microbiome Diversity
Physical activity independently improves gut bacteria diversity. Exercise increases blood flow to the digestive tract and stimulates beneficial bacterial growth. Active individuals show different microbiome compositions than sedentary people.

Moderate exercise provides optimal gut health benefits without overtaxing your system. Activities like brisk walking, cycling, or swimming support microbiome health. You don’t need intense workouts to see improvements.
Consistency matters more than intensity for gut health benefits. Aim for 30 minutes of moderate activity most days of the week. This regular movement pattern supports diverse, healthy gut bacteria populations.
Strategic Use of Probiotics and Supplements
Probiotic supplements can accelerate gut health recovery when used appropriately. These concentrated sources of beneficial bacteria provide targeted support beyond what diet alone can achieve. Understanding which strains address specific issues optimizes results.
Choosing Effective Probiotic Supplements
Not all probiotic supplements deliver meaningful benefits. Look for products containing well-researched strains at therapeutic doses. The most studied beneficial bacteria include Lactobacillus and Bifidobacterium species.

Colony-forming units (CFUs) indicate the number of viable bacteria in each dose. Effective supplements typically contain 10 to 50 billion CFUs. Higher doses aren’t necessarily better and may cause digestive upset in sensitive individuals.
Multi-strain formulas often outperform single-strain products. Different bacterial species perform different functions in your gut. A diverse supplement more closely mimics a healthy natural microbiome.
Complementary Supplements for Gut Support
Digestive enzymes help break down food when your body produces insufficient amounts. These supplements support nutrient absorption while reducing bloating and discomfort. They work particularly well for people with compromised digestion.
L-glutamine amino acid supports intestinal lining repair. This supplement helps restore gut barrier function in people with increased intestinal permeability. Research shows benefits for various digestive conditions.
Omega-3 fatty acids reduce inflammation throughout the digestive tract. Fish oil supplements provide concentrated anti-inflammatory compounds that support gut healing. They also promote beneficial bacteria growth.
Vitamin D influences gut bacteria composition and immune function. Many people with digestive issues show vitamin D deficiency. Supplementation may improve symptoms and support microbiome balance.
Discover the Complete Gut Restoration System
While individual strategies help, comprehensive gut health requires a systematic approach. This free presentation reveals the science-backed protocol that addresses all factors affecting your microbiome. Learn the exact steps thousands have used to transform their digestive health.
Foods and Substances That Harm Gut Health
Certain foods and additives actively damage your gut microbiome and intestinal lining. Identifying and minimizing these harmful substances accelerates your healing process. Small changes in what you avoid can produce significant improvements.
Processed Foods and Artificial Additives
Processed foods contain emulsifiers, preservatives, and artificial sweeteners that disrupt gut bacteria. These additives alter microbiome composition and increase intestinal permeability. The more processed your diet, the less diverse your gut bacteria.

Artificial sweeteners like aspartame and sucralose alter gut bacteria in ways that promote glucose intolerance. These sugar substitutes may actually increase metabolic problems rather than preventing them. Natural whole foods provide better alternatives.
Emulsifiers in processed foods break down the protective mucus layer in your intestine. This allows bacteria and toxins to contact intestinal cells directly, triggering inflammation. Avoiding packaged foods with long ingredient lists protects your gut barrier.
Sugar and Refined Carbohydrates
Excessive sugar consumption feeds harmful bacteria and yeast in your gut. These organisms outcompete beneficial bacteria when sugar is abundant. The resulting imbalance creates a range of digestive and systemic symptoms.
Refined carbohydrates behave like sugar in your digestive system. White bread, pastries, and other processed grains spike blood sugar and feed opportunistic gut bacteria. They also lack the fiber that beneficial bacteria need.
Reducing sugar and refined carbs starves harmful microorganisms while encouraging beneficial species to thrive. Focus on complex carbohydrates from whole grains, legumes, and vegetables. These provide sustained energy without feeding gut dysbiosis.

Alcohol and Its Effects on Gut Bacteria
Alcohol damages the intestinal lining and alters gut microbiome composition. Even moderate drinking increases intestinal permeability and promotes harmful bacterial overgrowth. Chronic alcohol use severely disrupts gut health.

If you drink alcohol, limit consumption to occasional small amounts. Red wine contains polyphenols that may offer some benefits, but alcohol’s negative effects generally outweigh these compounds. Water, herbal tea, and kombucha provide better beverage options.
Testing and Monitoring Your Gut Health Progress
Objective measurements help you understand your current gut health status and track improvement over time. Various testing options provide insights into bacterial composition, digestive function, and inflammatory markers. This data guides more targeted interventions.
Available Gut Health Testing Options
Comprehensive stool testing analyzes your gut microbiome composition and identifies specific bacterial imbalances. These tests measure beneficial bacteria levels, opportunistic organisms, and markers of inflammation. Results reveal which interventions will likely help most.

Food sensitivity testing identifies immune reactions to specific foods. Many digestive symptoms stem from unrecognized food sensitivities that trigger inflammation. Elimination diets based on testing results often produce dramatic improvements.
Breath tests diagnose small intestinal bacterial overgrowth and carbohydrate malabsorption. These conditions commonly contribute to bloating, gas, and irregular bowel movements. Identifying these issues allows for targeted treatment.
Tracking Symptoms and Progress
Maintaining a detailed symptom journal reveals patterns and triggers. Record what you eat, stress levels, sleep quality, and any symptoms you experience. Over time, this information highlights which factors most affect your gut health.
Track bowel movement frequency, consistency, and any associated discomfort. The Bristol Stool Scale provides a standardized way to assess stool quality. Changes in these patterns indicate how your gut is responding to interventions.
Monitor energy levels, mood, and cognitive function alongside digestive symptoms. Improvements in these areas often signal gut health restoration even before digestive symptoms fully resolve.
Regular progress reviews help you identify which strategies produce results. Compare your current symptoms to your baseline every few weeks. This reinforces positive changes and highlights areas needing adjustment.
Photography can document skin improvements related to gut health changes. Many people see dramatic skin clearing as their gut heals. These visual records provide motivating evidence of progress.
Natural Remedies and Therapeutic Approaches
Traditional healing systems have long recognized the importance of digestive health. Many natural remedies support gut healing through multiple mechanisms. These time-tested approaches complement modern interventions.
Herbal Medicines for Gut Support
Peppermint oil reduces symptoms of irritable bowel syndrome and calms digestive spasms. Enteric-coated capsules deliver the oil to your intestines where it provides therapeutic effects. Research consistently shows benefits for abdominal pain and bloating.

Ginger reduces nausea and supports digestive motility. This warming herb decreases inflammation in the digestive tract and may help balance gut bacteria. Fresh ginger tea or supplements both provide benefits.
Slippery elm creates a soothing coating on the intestinal lining. This traditional remedy relieves irritation and supports tissue healing. It works particularly well for people with inflammatory bowel conditions.
Bone Broth for Gut Healing
Bone broth contains gelatin and amino acids that support intestinal lining repair. The collagen in properly prepared broth helps seal a compromised gut barrier. Many people notice reduced symptoms after regularly consuming bone broth.
Making bone broth involves simmering animal bones for extended periods. This extracts beneficial compounds that aren’t available from muscle meat alone. The resulting liquid provides concentrated gut-healing nutrients.
Drink bone broth daily during active gut healing phases. It can replace other beverages or serve as a base for soups and stews. The warm liquid soothes your digestive tract while delivering therapeutic compounds.

Aloe Vera for Digestive Inflammation
Aloe vera juice reduces inflammation throughout the digestive system. This plant contains compounds that soothe irritated tissues and support healing. Look for products specifically formulated for internal use.

Start with small amounts of aloe juice and gradually increase as tolerated. Some people experience loose stools initially. Choose decolorized aloe products to avoid compounds that can irritate the intestine.
Building Sustainable Gut Health Habits
Long-term success requires integrating gut-healthy practices into your daily routine. Temporary changes produce temporary results. Creating systems and habits ensures continued benefits long after your initial improvements.
Meal Planning for Consistent Gut Support
Planning meals in advance removes the decision fatigue that leads to poor food choices. Dedicate time each week to plan gut-healthy meals and prepare key components. This investment pays dividends in consistent nutrition.

Stock your kitchen with gut-healthy staples that make nutritious meals convenient. Keep frozen vegetables, canned beans, whole grains, and probiotic foods readily available. When healthy options are accessible, you’ll choose them consistently.
Batch cooking saves time while ensuring you have gut-supportive meals ready. Prepare large quantities of soups, stews, or grain dishes that store well. Having these options available prevents relying on gut-damaging convenience foods.
Creating Environmental Support
Remove tempting processed foods from your home environment. When harmful foods aren’t readily available, you won’t eat them impulsively. Replace these items with gut-healthy alternatives that satisfy cravings.
Organize your kitchen to make healthy choices easier. Place vegetables at eye level in your refrigerator. Store whole grains and legumes in visible containers. These small changes unconsciously guide better decisions.
Develop supportive routines around meals. Eat at consistent times each day to support your microbiome’s circadian rhythms. Practice mindful eating by sitting down and chewing food thoroughly.
Build accountability through social support. Share your gut health goals with family or friends. Consider joining online communities focused on digestive wellness. These connections provide encouragement during challenging periods.
Handling Setbacks and Challenges
Expect occasional setbacks as part of the healing process. Stress, travel, or illness may temporarily disrupt your progress. View these situations as learning opportunities rather than failures.

Have strategies ready for common challenging situations. When traveling, research gut-friendly restaurant options in advance. Pack probiotic foods and supplements to maintain your routine. Planning prevents stress-driven poor choices.
Practice self-compassion when you deviate from your gut health plan. One less-than-ideal meal doesn’t undo weeks of progress. Simply return to your healthy habits at the next opportunity without guilt or self-criticism.
Common Gut Health Mistakes to Avoid
Well-intentioned efforts sometimes backfire when people make common errors. Understanding these pitfalls helps you navigate your gut health journey more effectively. Learning from others’ mistakes accelerates your progress.
Rushing the Process
Many people expect dramatic improvements within days of changing their diet. Gut healing requires time as beneficial bacteria gradually repopulate your digestive system. Rushing with aggressive interventions often creates more problems.
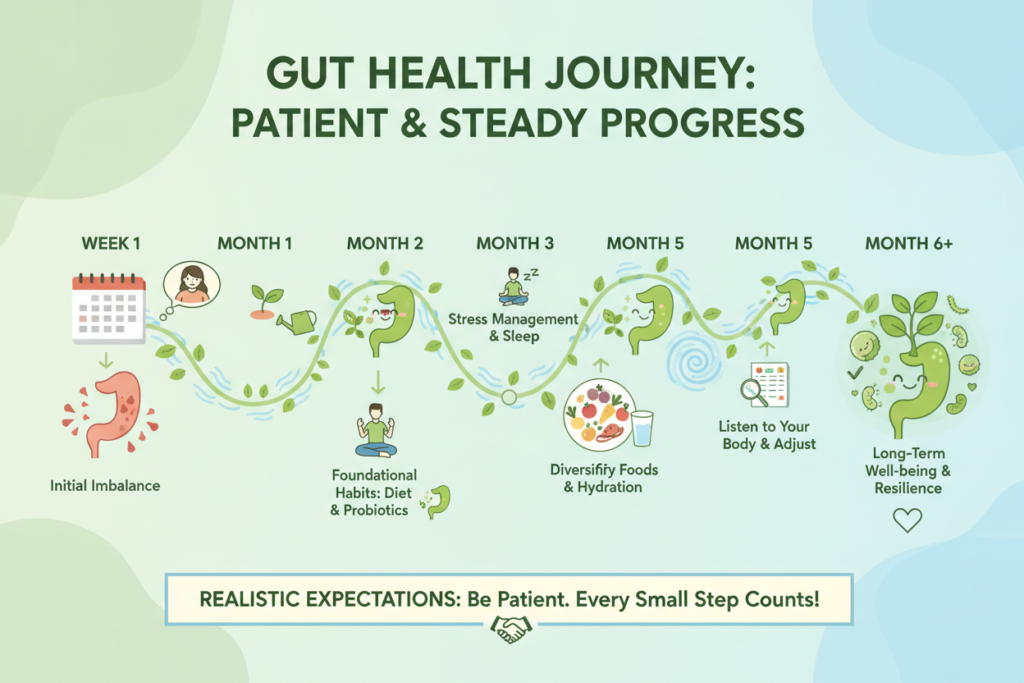
Introduce new foods and supplements slowly. Sudden dietary changes overwhelm your digestive system and cause uncomfortable symptoms. Gradual transitions allow your gut bacteria to adapt successfully.
Give each intervention adequate time before judging effectiveness. Most strategies require at least several weeks to produce noticeable results. Patience and consistency matter more than perfect execution.
Over-Relying on Supplements
Supplements support gut health but cannot replace a nutritious diet. Taking probiotics while continuing to eat processed foods yields limited results. Food provides the foundation while supplements offer targeted additional support.
Some people take excessive doses of probiotics assuming more is better. This can actually cause digestive upset and waste money. Follow recommended dosing and focus on quality rather than quantity.
Remember that supplements are meant to supplement, not replace, whole foods. Fruits, vegetables, and fermented foods provide benefits that isolated supplements cannot replicate. Prioritize real food first.
Avoid becoming dependent on digestive aids like enzymes or antacids for normal eating. While these can help during healing, the goal is restoring your body’s natural digestive capacity. Work toward gradually reducing reliance on these products.
Balance supplement use with lifestyle modifications. No pill can counteract chronic stress, poor sleep, or sedentary behavior. Address all factors affecting gut health for comprehensive results.
Ignoring Individual Responses
Generic gut health advice doesn’t work equally well for everyone. Your unique microbiome, genetics, and health history require personalized approaches. Pay attention to how your body responds to different interventions.
Foods that benefit most people may trigger symptoms in you. Keep detailed records of what you eat and how you feel. This data reveals your personal triggers and optimal foods.
Don’t persist with strategies that clearly aren’t working for you. If a particular probiotic strain or dietary approach causes worsening symptoms, try something different. Flexibility and self-awareness lead to better outcomes than rigidly following generic protocols.
Advanced Optimization Strategies
Once you’ve established basic gut health habits, advanced techniques can further optimize your microbiome. These evidence-based approaches target specific aspects of digestive function and bacterial balance.
Time-Restricted Eating for Gut Health
Limiting your eating to a specific daily window supports beneficial bacteria and gut barrier function. This approach, also called intermittent fasting, gives your digestive system extended rest periods. Research shows improvements in microbiome diversity and reduced inflammation.
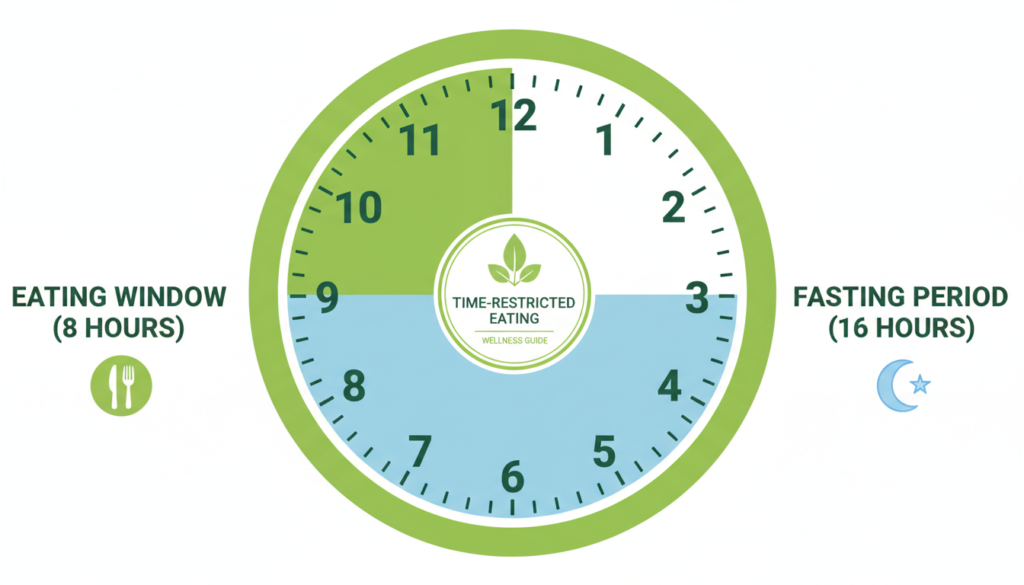
Start with a 12-hour eating window, such as 7 AM to 7 PM. Gradually narrow this to 10 or 8 hours as your body adapts. This pattern aligns with your gut bacteria’s natural circadian rhythms.
Time-restricted eating reduces late-night eating when digestive function naturally slows. This prevents undigested food from fermenting excessively in your intestine. Many people report reduced bloating and improved sleep quality.
Targeted Probiotic Rotation
Rotating different probiotic strains prevents dependency on specific bacteria. This strategy promotes broader microbiome diversity than taking the same supplement indefinitely. Switch between different multi-strain formulas every few months.
Consider soil-based probiotics as part of your rotation. These hardy bacterial strains survive stomach acid better than traditional probiotics. They may colonize your gut more effectively than standard Lactobacillus or Bifidobacterium supplements.
Take periodic breaks from probiotic supplements to assess your natural microbiome stability. If symptoms return during breaks, continue supplementation. If you maintain improvements without supplements, your gut may have achieved sustainable balance.

Polyphenol-Rich Foods for Microbiome Support
Plant polyphenols act as prebiotics while reducing inflammation. These compounds selectively feed beneficial bacteria and inhibit harmful species. Dark-colored fruits, vegetables, and beverages provide concentrated polyphenols.

Berries contain diverse polyphenols with potent gut health benefits. Blueberries, blackberries, and strawberries support beneficial Bifidobacteria growth. Aim for a serving of berries daily to maximize these effects.
Green tea provides catechins that reduce inflammation and support healthy gut bacteria. These compounds also enhance the gut barrier function. Drinking two to three cups daily offers measurable benefits without excessive caffeine.
Understanding the Gut-Brain Connection
Your gut and brain communicate constantly through neural, hormonal, and immune pathways. This bidirectional relationship means gut health affects mental wellness and vice versa. Addressing both systems simultaneously produces the best outcomes.
How Gut Bacteria Influence Your Brain
Gut microbiome produces neurotransmitters including serotonin, dopamine, and GABA. These chemical messengers directly affect mood, anxiety, and cognitive function. Approximately 90% of your body’s serotonin is manufactured in your gut.
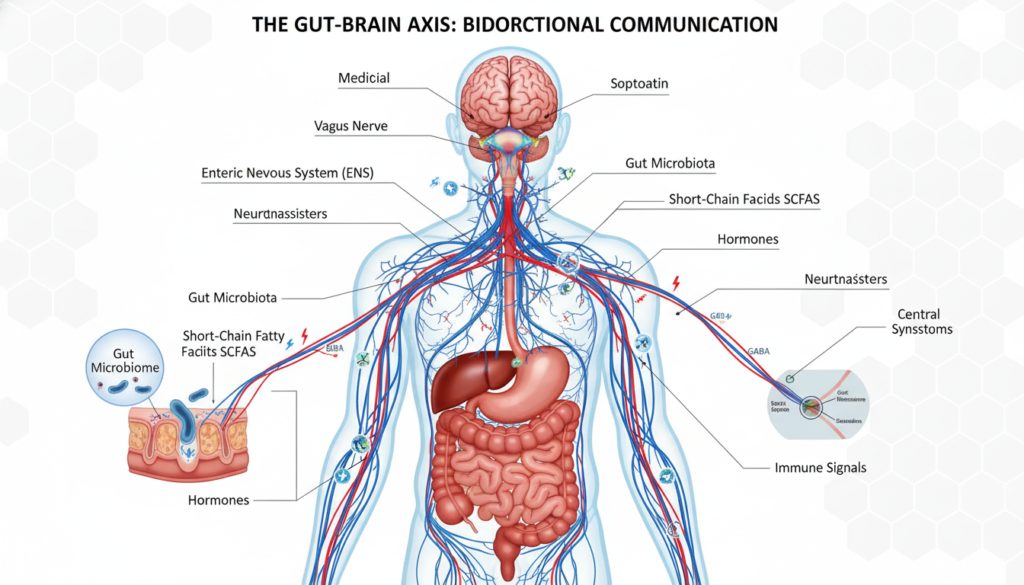
Bacterial metabolites enter your bloodstream and cross the blood-brain barrier. Short-chain fatty acids produced by gut bacteria influence brain function and protect against neurological conditions. Microbiome imbalances correlate with depression and anxiety disorders.
Improving gut health often resolves unexplained mood issues and brain fog. Many people report better mental clarity and emotional stability as their microbiome heals. This connection explains why digestive and mental health problems frequently occur together.
Managing Stress Through Gut Health
Chronic stress damages gut bacteria while gut dysfunction increases stress vulnerability. Breaking this cycle requires addressing both factors simultaneously. Gut-focused interventions can reduce stress sensitivity over time.
Specific probiotic strains show anti-anxiety effects in research studies. Lactobacillus rhamnosus and Bifidobacterium longum reduce stress hormones and improve stress resilience. These psychobiotic effects complement traditional stress management.
Mind-body practices like meditation and yoga benefit both gut health and mental wellness. These techniques reduce stress while supporting healthy gut bacteria through multiple mechanisms. Regular practice produces cumulative benefits.
Adequate omega-3 intake supports both brain function and gut health. These essential fats reduce neuroinflammation while promoting beneficial gut bacteria. Consider them foundational for mental and digestive wellness.
Long-Term Maintenance and Prevention
Achieving gut health represents only the beginning. Maintaining improvements requires ongoing attention to the factors that support your microbiome. Sustainable habits prevent regression and build resilience against future challenges.
Periodic Gut Health Check-Ins
Schedule regular assessments of your gut health status. Every few months, review your symptoms, energy levels, and overall wellness. These check-ins help you catch small problems before they escalate.
Consider annual comprehensive stool testing to monitor microbiome composition. These objective measurements reveal changes that may not produce obvious symptoms yet. Proactive monitoring allows early intervention when needed.
Adjust your approach based on life changes. Periods of high stress, travel, or illness may require temporarily intensifying gut support strategies. Flexibility in your maintenance plan ensures continued success.
Building Gut Health Resilience
A resilient gut microbiome bounces back quickly from temporary disruptions. Diversity in bacterial species creates this resilience. Continue eating a wide variety of plant foods to maintain microbiome diversity.
Occasional dietary indulgences won’t derail a well-established healthy gut. Once you’ve rebuilt robust bacterial populations, your microbiome can handle temporary deviations. This flexibility makes long-term maintenance sustainable.
Maintain your stress management and sleep practices even after digestive symptoms resolve. These lifestyle factors continuously influence gut health. Consistency in these areas prevents future problems.
Stay informed about emerging gut health research. Science continues revealing new strategies for supporting the microbiome. Incorporating evidence-based innovations keeps your approach current and effective.

When to Seek Professional Guidance
While many people successfully improve gut health through self-directed efforts, certain situations require professional evaluation. Recognizing when to seek expert help prevents unnecessary suffering and addresses underlying conditions.
Red Flag Symptoms Requiring Medical Attention
Severe or persistent abdominal pain demands professional evaluation. This symptom may indicate serious conditions requiring medical treatment. Don’t attempt to self-manage severe pain through dietary changes alone.

Unexplained weight loss alongside digestive symptoms requires investigation. This combination can signal inflammatory bowel disease or other serious disorders. Early diagnosis and treatment prevent complications.
Blood in stool, persistent vomiting, or high fever with digestive symptoms need immediate medical attention. These signs may indicate infections, inflammatory bowel conditions, or other acute problems requiring prompt treatment.
Working with Healthcare Professionals
Gastroenterologists specialize in digestive system disorders. These doctors can perform diagnostic testing and prescribe treatments for complex gut health issues. Consider consultation if symptoms persist despite dietary and lifestyle changes.
Functional medicine practitioners take a comprehensive approach to gut health. They often spend more time investigating root causes and may order specialized testing. This approach complements conventional gastroenterology.
Registered dietitians provide personalized nutrition guidance for digestive conditions. They can develop meal plans that address your specific needs and food sensitivities. Professional dietary support accelerates progress.
Mental health professionals should be consulted when gut issues significantly impact quality of life. The gut-brain connection means addressing psychological factors often improves physical symptoms. Integrated care produces the best outcomes.
Remember: Professional guidance doesn’t mean you’ve failed at self-care. Complex digestive issues often require expert support to fully resolve. Seeking help is a sign of wisdom, not weakness.
Your Path Forward: Taking Action on Gut Health
You now understand the multifaceted nature of gut health and the various strategies available for improvement. Knowledge alone changes nothing—consistent application of these principles produces results. Your gut microbiome responds to daily choices accumulated over time.

Start with foundational changes before attempting advanced strategies. Focus on increasing fiber intake, incorporating fermented foods, managing stress, and improving sleep. These basics provide the greatest return on your initial efforts.
Track your progress to maintain motivation and identify what works for your unique biology. Small improvements compound into dramatic transformations when sustained consistently. Celebrate each positive change rather than fixating on remaining symptoms.
Remember that gut health improvement is not linear. Expect fluctuations and temporary setbacks as part of the healing process. Persistence through challenges separates those who achieve lasting results from those who give up prematurely.
Benefits of Improved Gut Health
- Enhanced nutrient absorption and energy levels
- Reduced digestive symptoms like bloating and gas
- Stronger immune system function and disease resistance
- Improved mental clarity and emotional stability
- Better skin health and reduced inflammation
- Normalized bowel movements and digestive comfort
- Reduced risk of chronic diseases and disorders
- Enhanced overall quality of life and wellbeing
Common Challenges
- Initial adjustment period with dietary changes
- Requires consistent effort and lifestyle modifications
- Results may take weeks or months to fully manifest
- Individual responses vary requiring personalization
- Quality supplements and specialty foods can be costly
- Social situations may present dietary challenges
- Some symptoms may temporarily worsen before improving
- Requires patience during the healing process
While the strategies outlined in this guide provide substantial benefits, some people require more targeted support to achieve optimal results. Years of damage from antibiotics, processed foods, and chronic stress create complex imbalances that respond best to systematic protocols.
The cutting edge of gut health science has identified specific bacterial strains, precise dosing protocols, and strategic timing that accelerate healing. These research-backed approaches address the root causes of gut dysfunction rather than simply managing symptoms.
Transform Your Gut Health with Proven Science
You’ve learned valuable strategies for improving gut health through diet and lifestyle. Now discover the complete system that integrates these approaches with advanced probiotic science. This free presentation reveals the exact protocol that has helped thousands overcome chronic digestive issues and reclaim their health. Watch now to learn the breakthrough approach your gut has been waiting for.
Your gut health journey begins with a single decision to prioritize your digestive wellness. The information in this guide provides a solid foundation, but implementing it consistently determines your outcomes. Take action today on one or two strategies that resonated most strongly with you.
Your future self will thank you for the investment you make in gut health today. The ripple effects of a healthy microbiome extend to every system in your body. Start now, stay consistent, and trust the process as your body heals and rebalances.